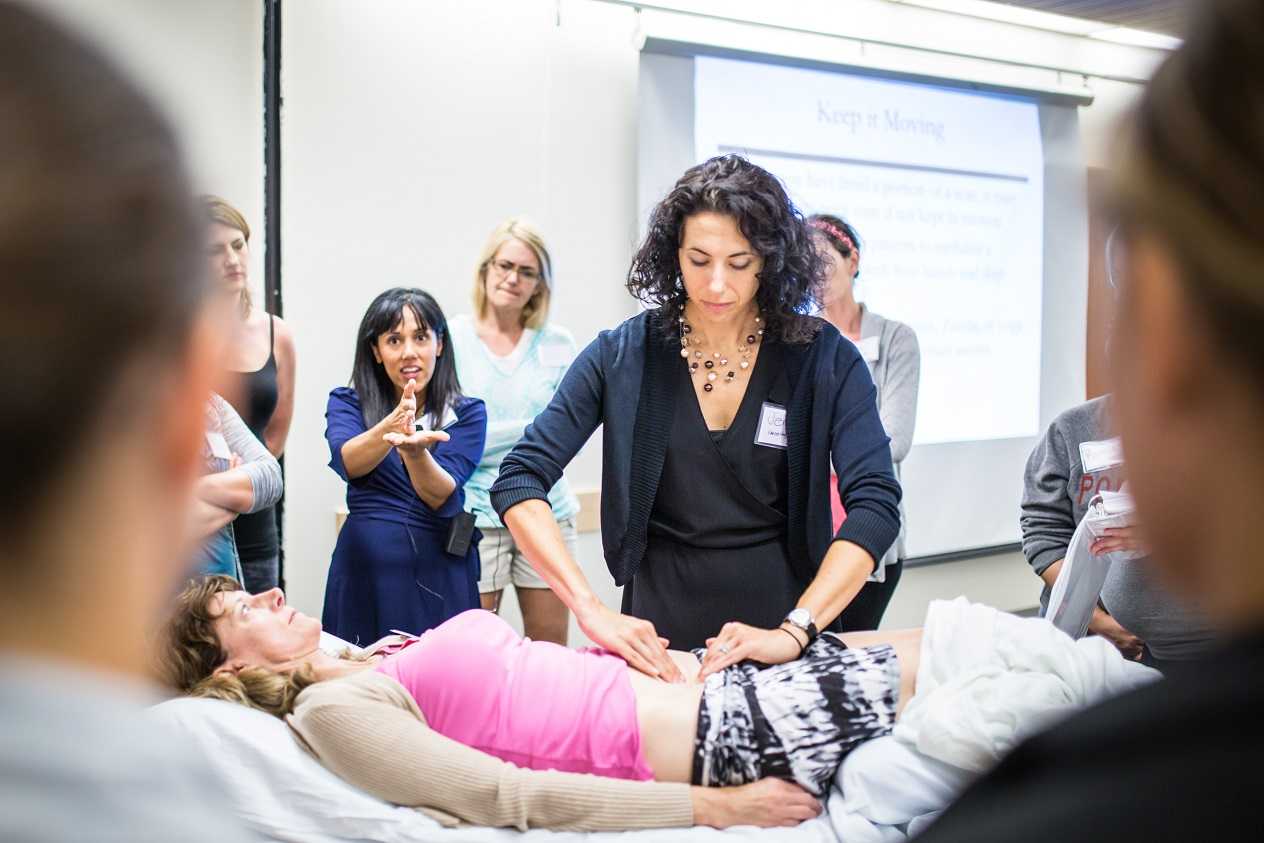
Ramona Horton, MPT, DPT developed and instructs the visceral and fascial mobilization courses for HW and presents frequently at local, national, and international venues – including International Pelvic Pain Society, CSM and HWConnect - on topics relating to women’s health, pelvic floor dysfunction, and manual therapy. Join Ramona in her upcoming course, Mobilization of the Myofascial Layer: Pelvis and Lower Extremity this February 2-4, 2024.
1. Learn from Ramona Horton!
Ramona C. Horton MPT, DPT serves as the lead therapist for her clinic’s pelvic dysfunction program in Medford, OR. Her practice focuses on treating adults and children with urological, gynecological, and colorectal issues. Her PT career began in the US Army, and she has taken the military “mission first” mentality into her approach to patient care. Simply said, “Diagnosis is just a label, perform a comprehensive musculoskeletal evaluation and treat what you find”. For her many contributions to the field of pelvic health, Ramona was awarded the prestigious Academy of Pelvic Health Elizabeth Noble Award in 2020.
2. The myofascial course is a concepts course.
The whole idea of the myofascial course is to help clinicians learn to problem-solve. To learn some basic concepts of physiology and mobility testing to stop chasing the boo-boo, and instead find and treat the cause. Just because it hurts at the right SI joint, doesn’t mean that you should treat the right SI joint. Joint hypermobility is profoundly nociceptive, especially in a one-bone/two-joint scenario as the sacrum and SI joints. Consider the idea that pain may be generated on the right from hypermobility that is a result of hypo-mobility on the left. Which side should then be treated, the painful side or the stiff side? Let’s treat where the brain is protecting and guarding the tissue.
3. Understand the true function and mechanisms of manual therapy.
Manual therapy is presented as a concept and technique that does NOT “release” tight or bound fascia based on the skill or magic hands of the practitioner. The issue is not in the tissue, if the tissue is tight, it’s tight because the brain is keeping it that way. Muscles are marionettes, and the brain is the puppet master. Manual therapy utilizes the fascial system to access the nervous system. In other words, having a conversation with the brain over the tissue that it appears to be protecting while trusting that the homeostatic mechanism is functioning in the body. If this is done in a non-threatening manner, the brain will normalize the tissue it is holding and guarding.
4. Add a whole host of new tools to your practitioner toolbelt.
The myofascial course teaches basic screening techniques that will point you in the right direction toward finding where the body is protecting, not where symptoms are being expressed. You will learn a variety of techniques to approach different fascial layers including direct and indirect fascial stacking for superficial nerves within the panniculus, muscular, and articular restrictions, as well as indirect technique of positional inhibition for trigger points. In addition, the science behind basic neural mobilization, instrument-assisted fascial mobilization and fascial decompression (cupping) are presented.
5. Learn more about fascia, its origins, and its functions.
Fascia is EVERYWHERE throughout the body; it is the ubiquitous connective tissue that holds every cell together much like the mortar in a brick wall, in addition to cells, it connects every system in the body. Fascia contains a vast neurological network including nociceptors, mechanoreceptors, and proprioceptors just to name a few. The fascial system has multiple layers within the body: starting at the panniculus which blends with the skin, the investing fascia surrounding muscles and forming septae, the visceral fascia which is by far the most complex and the deepest layer of fascia, the dura surrounding the central nervous system extending to the peripheral nerves. All fascial structures, regardless of layer or location have their origin in the mesoderm of early embryologic development. The myofascial course presents evaluation and treatment techniques for three of the four fascial layers while the three visceral courses address the complex visceral fascial layer.
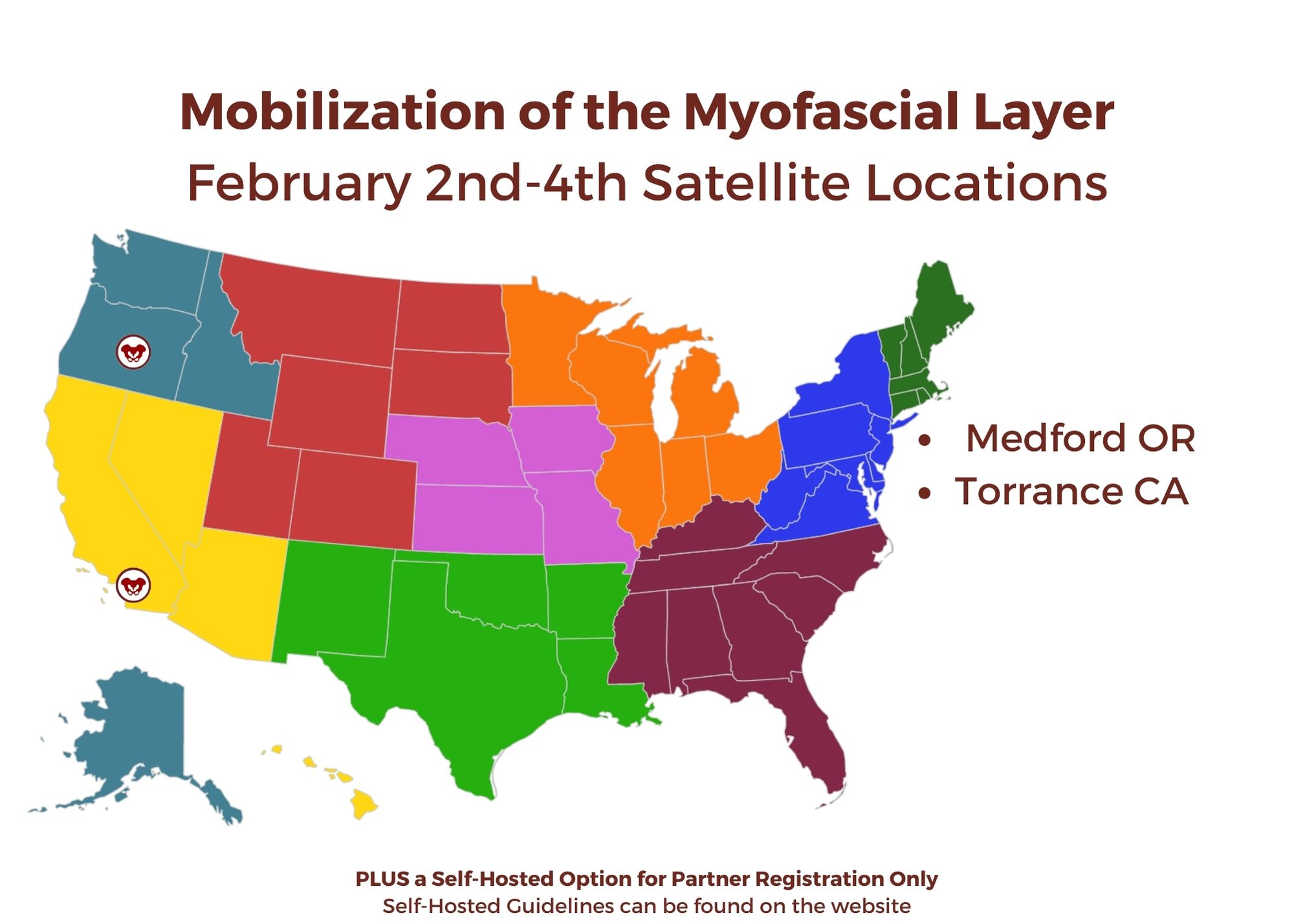
Mobilization of the Myofascial Layer: Pelvis and Lower Extremity
February 2-4, 2024
Price: $675
Experience Level: Intermediate
Contact Hours: 22.5
Medford, OR Satellite
Torrance, CA Satellite
Self-Hosted
HW Looks forward to seeing you in a future course!

We are pleased to announce the following changes and additions to our core series of courses. These changes are being undertaken by our Curriculum Development Team based on evolving realities of our field and the body of evidence and literature. In keeping with the way the field has evolved, we will be making the following changes to our core coursework.
Two courses will be joining our Pelvic Function Series:
- Pelvic Function Modalities - This brand new course is an in-person two-day continuing education course targeted to pelvic health clinicians covering frequently used modalities in pelvic health, including biofeedback and EStim. Hands-on labs using a variety of equipment necessitate that this course be offered in-person, where participants can practice using the equipment.
- Pelvic Function Level 2C: the Male Pelvic Floor and Men’s Pelvic Health - formerly the stand-alone course, Male Pelvic Floor Function Dysfunction and Treatment, this course is now being adapted and reformatted to be a part of the Pelvic Floor Series, reflecting the inclusive stance of H&W core series instructing in the care of all patients. This course will be offered as satellite, self-hosted, and in-person options in order to provide the most flexible pathway for participants.
In addition to these two new offerings, you will see greater inclusion of all genders throughout the series, starting with PF1. The modified titles and topics will be as follows:
Pelvic Function Level 1: Introduction to Pelvic Health - this course will provide a thorough and comprehensive introduction to anatomy and physiology of the pelvis and surrounding structures in all genders. Includes an introduction to performing intra-vaginal exam. This course will be offered in satellite and in-person formats.
Pelvic Function Level 2A: Colorectal Pelvic Health and Pudendal Neuralgia, Coccyx Pain. In labs, anorectal internal exam will be introduced. This course will be offered in satellite and in-person formats.
Pelvic Function Level 2B - Urogynecologic Topics in Pelvic Health. This course will be offered in satellite, self-hosted and in-person formats
Pelvic Function Series Capstone - Integration of Advanced Concepts in Pelvic Health. This course will remain targeted to the advanced clinician. A greater emphasis on workshopping clinical case studies will be incorporated. This course will be offered in satellite, self-hosted and in-person formats.
Questions:
What courses will be required in order to advance to the Capstone course?
As we understand the “advanced pelvic floor clinician” may have a variance of experience and focuses, the following course “journeys” can all be taken in order to take the Capstone course:
PF1
PF2A
P2B and/or PF2C
The Modalities course is strongly recommended, but not required, in order to take the Capstone course.
Why is the series being expanded and updated in this way? .
It is a reality of our field that pelvic rehab evolved from a tradition of “women’s health physical therapy”, and that is reflected in the vulvovaginal emphasis of the current coursework. As the scope of pelvic rehab has expanded to encompass men’s health and care for all genders, it is important that all pelvises be incorporated at every level of our series, and that men’s health be a foundational part of our curricula, rather than being siloed as a specialty offering.
I have already started my PF series coursework, where do I go now?
If you have taken only PF1, you should advance to PF2A, 2B or 2C in any order. You may also wish to take the Modalities course in order to learn evidence-based use of modalities and practice biofeedback and Estim in a hands-on, in-person setting. The best way to choose which course to take next will be determined by who shows up in your clinic after completing PF1 and beginning to see your first pelvic patient caseload.
If you have taken PF1 and 2A - take either 2B or 2C or both in any order to advance to Capstone. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs.
If you have taken PF1 and 2B, you must take 2A prior to Capstone. You may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs
If I have taken PF1, 2A, and 2B - you may advance to Capstone or you may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs
If you have taken PF1, 2A, 2B and Capstone but have not taken the former Male Pelvic Floor course, you may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals.
If you have taken PF1, 2A and the Male Pelvic Floor course, you may advance to Capstone
If you have taken PF1, 2A, 2B and the Male Pelvic Floor course, you may advance to Capstone
Am I required to take more courses in order to complete the PF series now?
No. Previously, there were three prerequisite courses for taking the advanced Capstone course: PF1, 2A and 2B. Following the changes to the series, the prerequisite courses for taking Capstone will be PF1, 2A and 2B OR 2C (or both, depending on one’s target patient population). The Modalities course is a strongly encouraged, but not required, level of the PF series.
As before, participants should choose their next course based on the patient needs they are seeing in the clinic. Following PF1, many may see patients with fecal incontinence or coccyx pain and may choose to prioritize PF2A as the next step in their journey. Others may see patients with penile pain or incontinence post-prostatectomy and may choose to take 2C as their next step.
As before, there are no required courses in order to sit for the Pelvic Rehab Practitioner Certification Exam.
Why aren’t there self-hosted options for PF1 and PF2A?
PF1 is most learners’ first introduction to performing intra-vaginal assessment and therefore we believe the best learning experience will be under the guidance of either an HW faculty member or trained teaching assistant at an in-person or satellite course. Similarly, PF2A is most learners’ first experience performing anorectal exam, which should also take place under the supervision of an experienced clinician. In PF2B, 2C, and Capstone, these techniques are refined and it is therefore appropriate to allow self-hosted options for those who have already learned these skills and are comfortable with independent learning.
I see that there will be options for a few in-person as well as satellite offerings for much of the series. Will HW continue to offer both formats?
We understand that many people appreciate the flexibility and accessibility of the satellite model as an improvement over the days when all series courses were sold out with long waitlists and lengthy travel was often required to attend our courses. We also understand that some folks simply prefer the format in which instructors are present at the course. Our intention is to offer formats that accommodate everyone’s needs, which is why the PF series will be available in-person as well as in the satellite format starting in 2024. Because of the hands-on equipment needs of the Modalities course, this will be available exclusively in person.
Why is PF1 required for 2C if it wasn't for MPF?
Historically, the Male Pelvic Floor course was a stand-alone course, meaning that many participants would take this course after beginning their journey with PF1 and after already seeing patients with pelvic floor dysfunction. Others, often male and male-identifying practitioners who did not feel their goals were met by the vulvovaginal-centered PF series, would take the Male course as their first ever introduction to pelvic health. This resulted in course attendees being in vastly different places in terms of experience, which often results in a sub-optimal learning experience for all.
As part of our push to see more information about patients of all genders incorporated at every level of the core series, PF1 which contains foundational information on all pelvises and core concepts in pelvic rehab, will be a prerequisite for 2C, which will build on those core concepts as they apply specifically to the male and male-identifying patient.
Who can act as a Teaching Assistant for the series courses in the new format?
PF1 - must have PF1, and ⅔ of the Level 2s (2A, 2B, and 2C)
PF2A - must have 1, 2A, and 2B or C
PF2B - must have 1, 2B
PF2C - must have 1 and have taken the Male Pelvic Floor in 2016 or later
Capstone - must have 1, 2A, 2B or 2C, and Capstone

Senior faculty member Allison Ariail, PT, DPT, CLT-LANA, BCB-PMD, PRPC sat down with the Pelvic Rehab Report to talk about the role pelvic therapists play on the oncology team that will work with the patient throughout treatment and into survivorship and the impact pelvic health has on quality of life for people with cancer.
Alison is part of the HW faculty team that wrote and instructs the Oncology course series, the next course is Oncology and the Pelvic Floor Level 1 on January 27-28, 2024.
Did you know that there are over 15 million cancer survivors in the United States? As advancements in care and early diagnosis improve, this is expected to increase to over 20 million survivors in the next 10 years. The continuum of care for patients with cancer ideally begins at diagnosis and the rehabilitation professional is an integral part of the oncology team that will work with the patient throughout treatment and into survivorship.
Pelvic cancers can include bladder cancer, cervical cancer, colorectal cancer, ovarian cancer, prostate cancer, and uterine cancer, among others. These patients can experience changes in how their body functions during or after cancer and its treatment. Changes caused by the treatment of cancer can lead to pain, discomfort, and problems with bowel, bladder, and sexual function
Why did you become a pelvic therapist?
I was attracted to pelvic therapy because I enjoy helping people who aren’t getting the help they need from other sources. When I first started working in pelvic floor therapy, there were not as many therapists working in the field. I absolutely loved it! I really enjoyed seeing the improvements patients made and the excitement that they had when they could come in and share with me that they saw improvements. They would share with me news about bowel, bladder, or sexual function that they would not even share with their partner. To see the happiness that people had with improvements in this intimate part of their lives really brought me joy. I enjoy helping people have hope in their lives and working with these patients is very rewarding to me.
What role does a rehab practitioner play on the oncology team?
Rehab professionals are key members of the oncology team. While the other members of the oncology team are focused on curing the cancer and helping the patient live longer, rehabilitation professionals focus on getting the patient to be able to do things in their lives that they enjoy. We are trained in working with the body and identifying dysfunction within the body that is limiting the patient and keeping them from functioning to their full potential. We have skills to address the musculoskeletal, visceral, nervous, and integumentary systems that can help improve the way a patient’s body is working and therefore improve function. Sometimes we address the little things with patients that then make the biggest impact in them living their lives. One patient of mine said that “her doctors saved her life, but her therapist helped her put her life back together so she could live it.” This quote really demonstrates the role a rehabilitation professional can have on an oncology patient.
What are some of the most important things you (and pelvic therapists) do for people with cancer in your role?
One of the most important things we therapists can do for our oncology patients is to listen. We spend a lot of time with our patients and develop a rapport with our patients. They then often share things with us they may not other providers. We have the skills to treat and help our patients with very personal symptoms in intimate areas. Pelvic floor therapists can help oncology patients return to a life that is more similar to their life before their cancer diagnosis. This is important. Their lives have been changed forever with their cancer diagnosis. If we can listen to the patient, and improve some of the symptoms they are experiencing; it can make a bigger difference than we think in helping them return to living their lives.
What are some common concerns oncology patients have, and how do you help address them?
One of the biggest issues oncology patients experience is restricted movement within the body. Surgery, and radiation both cause changes to the body that lead to scarring, fibrosis, and adhesions. This leads to a tightness that limits the normal movement of a body part, or decreased glide of the tissues. We address this a lot in the oncology series. We learn how to work with this restricted movement and help improve it. If the rehabilitation clinician can improve the ability of the body to move (whether it is a joint, a muscle, or the glide within the tissues), then this can ease pain, improve the function of that body part, and improve overall mobility and function for the patient.
What is the number one thing that practitioners should be aware of when it comes to pelvic therapy and cancer?
Radiated tissue is never the same as before it was radiated. Even if it has been years. Radiation changes the tissues. It can lead to inflammation, fibrosis, scarring, adhesions, texture change, and elasticity changes, among other effects. The effects of radiation can continue for years, and the tissues should be treated differently even if it has been many years since the patient underwent radiation. The therapist should learn to “listen” with their hand to see what state the tissues are in, and how to treat these tissues in a gentle and non-aggressive manner.
How can people with cancer better communicate with their pelvic therapists, and how can the practitioner facilitate these conversations?
I would encourage any cancer survivor to tell their therapist what is keeping them from doing what they love. When someone is diagnosed with cancer and goes through treatment, they often become limited in some of their activities. Unfortunately, many people don’t return to the activities that brought them joy. I would encourage patients to tell their therapist things that they wish they could do but cannot. Even if it is something little like making the bed, cooking a meal, or walking to the bathroom without leaking. Or if it is something bigger, like jumping on the trampoline with their kids, or returning to their exercise routine.
The therapist needs to know what it is that the patient would like to do but cannot do at this time. That way we can analyze the situation and figure out what can be done to help the patient reach their goal. I encourage therapists to ask their patients “What do you wish you could do but can’t now?”, or “What activities bring you joy?” If they are not able to do these activities after cancer treatment, work with the patient to see if you can help them return to that activity. It may be in baby steps, but that still can bring the patient joy!
What are some of the most rewarding parts of your job?
What I enjoy most about my job and working with oncology patients is the hope that I get to experience alongside these patients. I have the privilege of being able to work with these fighters and help them to gain function. The happiness they have when they can return to a loved activity, have an orgasm again, or be able to go to a movie without having fecal urgency is so very rewarding. I work with patients and try to instill an optimism that they can return to a better state. However, they also give me hope in life. Seeing their perseverance, their will to live, and their fight is inspirational! Working with oncology patients provides a positive light in my life; knowing that I am helping people that really need it, and the inspiration I get from working with these patients is amazing!
Join Oncology and the Pelvic Floor Level 1 on January 27-28, 2024 to learn more about working with oncology patients as part of an interdisciplinary oncology team to improve patient outcomes and quality of life.

Kristina Koch, PT, DPT, WCS, CLT is a board-certified clinical specialist in women’s health physical therapy and a certified lymphedema therapist. Kristina has been treating pelvic health conditions in individuals of all ages and genders since 2001 and works in private practice in Colorado Springs, CO. Kristina is a member of the HW faculty with her own course, Pharmacologic Considerations for the Pelvic Health Provider, scheduled next on February 4, 2024.
Why it is Important to Know Pharmacology
All rehab providers need to have a foundational understanding of pharmacology for numerous reasons, all of which contribute to providing safe, effective, and comprehensive care to their patients. In pelvic health, therapists often encounter patients who are taking numerous medications, and it is important for us to understand how these drugs may impact a patient's physical function, exercise tolerance, current complaints, and overall well-being.
Basic pharmacology knowledge includes:
- Understanding drug classes
- Pharmacokinetics and pharmacodynamics: how drugs exert their effect on the body and how the body impacts the drug
- Drug interactions: recognizing potential interactions between medications and how they may affect a patient's response to therapy interventions.
- Adverse Effects: awareness of possible side effects of medications that could impact a patient's ability to participate in therapy or contribute to their symptoms.
A more comprehensive understanding of pharmacology has clinical relevance on many fronts. The following bullet points highlight how understanding pharmacology has implications for clinical practice.
Assessment:
Pharmacological knowledge allows clinicians to conduct a more comprehensive assessment of their patients. Considering a patient's medication history as part of the overall health profile helps clinicians tailor treatment plans to individual needs and potential limitations.
Safe and Effective Patient Care:
Rehab providers often work with patients who are taking medications for various health conditions. Understanding pharmacology enables therapists to assess potential interactions between drugs and design safe and effective treatment plans.
Optimizing Rehabilitation Strategies:
Medications can impact a patient's response to exercise and rehabilitation. Understanding pharmacology enables rehab providers and therapists to modify treatment plans based on a patient's medication profile, potentially optimizing rehabilitation outcomes.
Pain Management:
Pain is a common reason our patients are seeking physical therapy. Knowledge of medications used for pain management enables therapists to collaborate with healthcare providers to create comprehensive pain management strategies for their patients.
Collaborative Care:
Clinicians often collaborate with physicians, nurses, and other healthcare providers. Knowledge of pharmacology facilitates effective communication, allowing therapists to discuss patient cases, contribute to treatment decisions, and foster a collaborative approach to patient care.
Educating and Empowering Patients:
Pelvic health practitioners and rehab providers play a vital role in educating patients about their health, including medications. Understanding pharmacology allows therapists to explain the purpose of medications, potential side effects, and the importance of compliance, encouraging patient engagement and adherence to treatment plans.
Recognition of Red Flags:
Knowledge of pharmacology enables pelvic health rehab providers to recognize signs and symptoms of adverse drug reactions, identify potential issues early, consult with healthcare providers, and modify treatment plans accordingly.
Informed Decision-Making:
In certain situations, therapists and rehab providers may need to make decisions regarding treatment plans and goals, treatment frequency, or modalities based on a patient's medication profile. A solid understanding of pharmacology contributes to informed decision-making.
Legal and Ethical Considerations:
Pelvic health practitioners need to work within their scope of practice. An understanding of pharmacology helps therapists recognize when it is appropriate to refer patients to other healthcare professionals for medication management.
Monitoring and Reporting:
Monitoring patients for signs of adverse reactions and knowing when to report concerns to other healthcare professionals or federal organizations.
Special Populations:
Pediatrics and geriatrics may require special consideration due to differences in pharmacokinetics and pharmacodynamics. Understanding how medications affect different age groups helps pelvic health therapists and rehab providers adapt our interventions accordingly.
As rehabilitation providers, we invest a substantial amount of time in direct interaction with our patients during their treatment sessions, surpassing the duration they spend with their primary care providers. This prolonged and more frequent engagement, spanning weeks or months, affords our patients an increased opportunity to communicate not only their physical concerns but also their apprehensions regarding medications and potential side effects. This dialogue exceeds what may occur with their physicians or primary care providers. Understanding the impact of medications on a patient is vital for effectively educating them about potential side effects and how these medications may contribute to their complaints, thereby augmenting the overall value of the treatment regimen.
With a solid grasp of pharmacology and insight into medications prescribed for pelvic health, therapists can engage in informed discussions with patients and collaborate effectively with other healthcare providers involved in their care. The capability to explore recent medications, supplements, or alternative approaches that may minimize side effects, mitigate impacts on quality of life, and enhance function. Remaining current on advancements in pharmacology is indispensable for delivering physical therapy interventions that are both effective and grounded in evidence-based practices.
In summary, a strong understanding of pharmacology enhances the overall quality of physical therapy practice. It ensures that physical therapists and rehab providers can provide patient-centered, evidence-based care while collaborating effectively within the broader healthcare team.
Join Kristina in Pharmacologic Considerations for the Pelvic Health Provider on February 4, 2024, to learn about the medications frequently used in pelvic health, their side effects, the clinical impact they may have on your patients, and possible alternatives to consider to improve patient outcomes and quality of life.

Megan Pribyl, PT, CMPT is a practicing physical therapist at the Olathe Medical Center in Olathe, KS treating a diverse outpatient population in orthopedics including pelvic rehabilitation. Megan’s longstanding passion for both nutritional sciences and manual therapy has culminated in the creation of her remote course, Nutrition Perspectives for the Pelvic Rehab Therapist, designed to propel understanding of human physiology as it relates to pelvic conditions, pain, healing, and therapeutic response.
She harnesses her passion to continually update this course with cutting-edge discoveries creating a unique experience sure to elevate your level of appreciation for the complex and fascinating nature of clinical presentations in orthopedic manual therapy and pelvic rehabilitation.
Indulgences over the holiday season lead many to experience symptoms of indigestion, part of the discomfort that fuels our renewed January focus on exercise and “eating right”.
With this in mind, let’s discuss how we as a nation handle GI distress or GERD (gastroesophageal reflux disease) symptoms. Typically here in the US, there are 2 methods we typically use:
- The quick way - by popping a Tums or Rolaids or
- The prolonged way - by taking PPI’s (proton pump inhibitors) or H-2 blockers on a regular basis (eg. Pepcid AC).
Both are reliable ways to efficiently feel a little less GI distress.
The quick relief strategy neutralizes the acid that is already in the stomach whereas the longer-acting PPI’s and H-2 blockers actually block or suppress acid production in the stomach. And even though these “longer term” drugs are designed for short-term use, the more I inquire about their use with my patients, the more a troublesome pattern emerges. Many of my patients struggling with complex symptom constellations (eg. a non-relaxing pelvic floor, constipation, perineal skin issues, gut issues, anxiety, depressive symptoms, etc.) describe that they have taken these “digestive aides” continually for years. YEARS.
So, this approach is fine, yes? We know acid reflux can lead to esophageal irritation, not to mention pain and nagging discomfort. It can lead to disordered sleep and its associated sequelae. In extreme cases, esophageal irritation could even progress to esophageal cancer. Therein lies the justification for using drugs that suppress or block acid production in the stomach over the long term. Even though long-term safe use of these drugs has never been established.
Hmmm. I hope this is cause for pause. It’s true we don’t want GERD or indigestion, yet it remains ubiquitous. The prevalence of at least weekly GERD symptoms in the US is approximately 20% (El-Serag et al., 2014) with an overall prevalence estimated up to 30% in the US (Eusebi et al., 2017). This prevalence of GERD is deemed “exceedingly common”, ranking as the most frequent gastrointestinal diagnosis associated with outpatient clinic visits in the US (Richter, 2018). For as frequently as I see these drugs listed on patient intake forms - or forgotten to be listed since it is such a part of one’s routine - I feel strongly that we are dealing with an epidemic I call “indigestion nation”.
Instead of blaming our stomach acid, it’s time for us to look at the other side of the issue and ask why. Why are so many struggling with digestion? And is there a better way to get a handle on this under-appreciated situation?
Next question: how often is nutrition or food digestibility considered in scenarios involving GERD symptoms, GI upset, or indigestion?
When I ask my patients about this, the standard answer prevails: they try their best to avoid known triggers including fried and spicy foods. Beyond that, there is little forward thinking in terms of where our collective indigestion originates.
Further, how many healthcare providers or patients contemplate what long-term acid suppression might look like?
- Isn’t our stomach SUPPOSED to be acidic? (Answer: it is)
- What happens if it isn’t? (Answer: lots of undesirable things)
- From there, we begin connecting the dots to find points of clarity.
In order to digest proteins, our stomach has to be acidic. The acid in the stomach also kills or deactivates harmful viruses and bacteria that could otherwise gain access to the rest of our system via the intestinal barrier. And our standard American diet does not include foods that contain important bioactive compounds and enzymes that take some of the burden of digestion off our plate – or rather our stomach, intestines, and accessory digestive organs. These are not frequently discussed principles of digestion.
We are conditioned to seek the quick fixes to our digestive woes. Woes that have increased in prevalence in North America by approximately 50%, relative to the baseline prevalence in the early to middle 1990s (Richter, 2018). Our go-to quick (Tums and Rolaids) and long-term strategies (Pepcid AC) are not without consequences. And I’m not even referring to the recently elucidated serious issue of the H-2 blocker ranitidine (generic Zantac) containing N-nitrosodimethylamine (NDMA)….a probable human carcinogen (Mahase, 2019).
Facts like these will sometimes get us to take notice. However, the more pervasive problem is this: components of our diets have become so difficult to digest, so physiologically incompatible with us, that we forget to examine this issue through such a simple lens. If our diet consists of foods that are difficult to break down or contain substances that can be disruptive to our digestive processes, it’s no surprise our body may reject them or be unable to digest them fully.
However, if our diet consists of foods that are designed for nourishment, naturally pre-digested and ready to assimilate or use by the body for building blocks and fuel, our body will know how to break them down and utilize them fully…..miraculously reducing the digestive burden and improving symptoms of GI distress including GERD and indigestion.
It sounds simple enough.
But in this day and age, the savvy healthcare provider will do well to learn and appreciate the breadth and depth of this concept and what it means to you as both a consumer of food and one who cares for others who consume food - all of us. This understanding - especially for a pelvic rehab provider- is critical to harness.
From simple but nuanced concepts, one can help prompt remarkable changes. I’ve seen it firsthand innumerable times.

I invite each of you to learn more about this fascinating topic and how it interrelates with so many facets of our health. Take advantage of the multiple remote-course offerings of Nutrition Perspectives for the Pelvic Rehab Therapist in 2024 - February 24-25, April 27-28, June 8-9, and December 7-8.
References:
- Richter, J. E., & Rubenstein, J. H. (2018). Presentation and Epidemiology of Gastroesophageal Reflux Disease. Gastroenterology, 154(2), 267-276. doi:10.1053/j.gastro.2017.07.045
- Eusebi LH, Ratnakumaran R, Yuan Y, et al. Global prevalence of, and risk factors for, gastro- oesophageal reflux symptoms: a meta-analysis. Gut. 2017
- El-Serag HB, Sweet S, Winchester CC, et al. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2014; 63(6):871– [PubMed: 23853213]
- Mahase, E. (2019). FDA recalls ranitidine medicines over potential cancer causing impurity. BMJ, 367, l5832. doi:10.1136/bmj.l5832

HW is excited to announce the addition of a brand-new course to our Pelvic Function (PF) Series!
Pelvic Function Level 2C (PF2C): the Male Pelvic Floor and Men’s Pelvic Health
Formerly the stand-alone course, Male Pelvic Floor Function Dysfunction and Treatment, this course is now being adapted and reformatted to be a part of the PF Series, reflecting the inclusive stance of H&W core series instructing in the care of all patients. This course is intended for the pelvic health clinician who treats patients with conditions including post-prostatectomy urinary incontinence, erectile dysfunction, and chronic pelvic pain (CPP).
This course will be offered as satellite, self-hosted, and in-person options in order to provide the most flexible pathway for participants.
It is a reality of our field that pelvic rehab evolved from a tradition of “women’s health physical therapy”, and that is reflected in the prior vulvovaginal emphasis of the existing coursework. As the scope of pelvic rehab has expanded to encompass men’s health and care for all genders, it is important that all pelvises be incorporated at every level of our series, and that men’s health be a foundational part of our curricula, rather than being siloed as a specialty offering.
It is now our expectation that providers who want to care for patients around topics provided in the men’s health course will now take our introductory course, Pelvic Function 1. This is a necessary change reflecting growth and progression of our field of pelvic healthcare. Over the years, it was helpful to offer a course focusing on post-prostatectomy dysfunction, pelvic and genital pain and sexual health and function that was open to all levels. However, while participants who took the former Male Pelvic Floor course developed competence in the instructed skills, by missing the rest of the series, foundational conversations including physiology of urinary function, discussion of trauma-aware care, and bowel health basics that often affect other pelvic functions were abbreviated. Including men’s health within the rest of the foundational series resolves the missed content from our foundational course. Attendees to our PF1 course will find that it has been elevated to be a more inclusive course that covers information about pelvic health which will allow a beginning pelvic health practitioner to immediately apply introductory principles of care to all genders.
More questions about changes to the PF series? Please see this FAQ page: https://hermanwallace.com/frequently-asked-questions#2024-PF-Series-Update

Within the walls of the pelvic rehabilitation clinics, we often hear more intimate details than we ever imagined we would, could, or perhaps should. With increasing patient care experiences, most therapists demonstrate increased knowledge, awareness, and with some practice, increased skill at discussing sensitive issues such as sexuality. Every person and relationship is unique and we are sometimes asked questions by our patients such as "Should I be having more sex?" or "Am I normal?"
I have sometimes been surprised when a patient reports that he or she is "not having sex often enough" and for that patient it means that daily sexual activity is no longer happening. Other patients are quite satisfied with their sexual activity occurring 2-3x/month. We meet patients who have gone for years without engaging in sexual activity, perhaps because of pain, or lack of intimate partnership, or medical issues with a partner. It is very useful to avoid having expectations for what we as therapists think a patient should or should not be doing, whether that pertains to a particular sexual practice or to a level of involvement with a partner.
-Holly Tanner. Sexuality and the Older Patient. Tuesday, 13 September 2011.
Herman & Wallace offers several course options that deal with these sexual topics. Those courses that have upcoming course dates are:
Enjoy a 10% discount on these 3 courses if you register between now and midnight Wednesday, December 6th, 2023 with coupon code: SEXED10
Application Fee: $375.00 Experience Level: Beginner Contact Hours: 12
Course Date: December 9-10, 2023
It is vital that providers working with pelvic floor concerns have the necessary education and training to work with patients on issues of sexual dysfunction. It is also important that providers be aware of their own biases and be introduced to the various sexual health resources available to providers and patients.
Sexuality is core to most human beings’ identity and daily experiences. When there are concerns relating to our sexual identity, sexual health, and capacity to access our full potential, it affects our quality of life as well as our holistic well-being. Working with folks on issues of sexual health and decreasing sexual dysfunction encourages awareness and encourages healing. Imagining a world where human beings don’t walk around holding shame or traumatic pain is imaging a world of health and happiness.
Often unwanted sexual pain goes unaddressed. Why? Because we are not taught about the interactions between feelings, relationships, and our body. We are not taught that sex should not be painful; that pain is (likely) our body giving us information that something is going on (Hello crappy sex education and the stigma of sexual health and body awareness!). It’s not uncommon that most people who experience sexual pain often feel they are broken.
How to heal from unwanted sexual pain? There’s a trifecta! Effective healing comes from working with a sex-positive medical provider, sex therapist, and pelvic floor therapist. We will all collaborate!
Sex is not supposed to be painful. You are not broken.
Sexual Interviewing for Pelvic Health Therapists is two day course, written and instructed by a Licensed Marriage and Family Therapist and AASECT Certified Sex Therapist and is intended for pelvic rehab therapists who want to learn tools and strategies from a sex therapist’s toolkit. Lecture topics include bio-psycho-social-spiritual interviewing skills, maintaining a patient-centered approach to taking a sexual history, and awareness of potential provider biases that could compromise treatment. Labs take the form of experiential practice with Bio-Psycho-Social-Spiritual-Sexual Interviewing Skills, case studies and role playing.
Upon completion of this course, participants will be able to provide a Comprehensive Sexual Health Interview, recognize potential biases when working with patients, identify ethical considerations, and effectively collaborate with behavioral health providers upon referral. This course is intended for participants in the medical profession who work with patients experiencing pelvic pain, pelvic floor hypertonicity, and other pelvic floor concerns.
-Mia Fine. Pain during sex? It might be Dyspareunia. Tuesday, 18 May 2021.
Application Fee: $275.00 Experience Level: Beginner Contact Hours: 9.75
Course Date: January 7, 2024
CASE STUDY: Sarah is a 23-year-old woman who presents to your office for an evaluation. Upon scheduling, she did not wish to disclose to your office manager what kind of pelvic health issue she wants to be seen for.
Upon patient interview, Sarah reveals that she has been married for 8 months and all attempts at intercourse have been unbearably painful. She reports a 14/10 on a pain scale and that she has vocally cried out in pain with any attempts at penetration. She is feeling hopeless that this will ever get better, and is concerned that something is wrong with her and that her vagina is “too small” for intercourse. Sarah admits that she has never examined her own vaginal opening or seen it in a mirror because it “grosses her out”.
Sarah is otherwise in good health but has never had a gynecological exam. She and her husband are both from a conservative religious background and were educated in religious schools with limited sex education, and were provided with little information about sex prior to marriage. Neither of them had been sexually active prior to marriage. Sarah currently ascribes to her religious beliefs and practice which prohibits any conversations about sex with anyone other than her partner. She expresses an aversion to sexual activity and to her husband’s genitalia and semen. Sarah confides that she feels guilty that she is not able to have intercourse and “make her husband happy”.
Although she denies any discomfort with sitting or wearing tight-fitted garments and has no other pain in her body, recently she has started to have pain in her vulvar area that starts before attempting intercourse. After attempts at penetration, she has difficulty falling asleep due to her pain.
She has a self-diagnosed “tiny bladder” and frequently has to urinate every hour. Sarah reports a long history of constipation, with bowel movements about once a week with straining (type 1-2 on the Bristol stool scale)
She reports regular periods, but excruciating pain the first 2-3 days that can be debilitating at times. She has never successfully inserted a tampon.
Sarah’s personal goals for treatment are:
- To have intercourse without pain
- To become pregnant as soon as possible, as is expected in her social circles and close-knit community
- What is your next move?
- What other questions would you like to ask this patient?
- What would your treatment plan look like for this patient?
- What other healthcare providers might you refer her to?
Sex and Religion has the following goals:
- Demonstrate a foundational understanding of the traditions, customs, laws, and values associated with different faiths.
- Identify potential challenges and barriers to care unique to pelvic health patients from conservative religious backgrounds.
- Describe five strategies for increasing comfort and confidence in interfacing with patients from different religious backgrounds.
- Patient interview and education techniques.
- Discuss collaborative approaches to evaluation and treatment that are compliant with the patient’s religious and cultural norms.
- Evaluate culturally sensitive intervention in a case study format with your peers.
As pelvic health providers, we go into this special field with the desire to provide the best care for our patients in the most sensitive way possible. It can be particularly daunting when we encounter patients from religious backgrounds and cultures that are unfamiliar to us. In our attempts to be sensitive, we may be tempted to shy away from asking patients the questions that really need to be asked. We may avoid providing patient education we may have otherwise provided because we don’t want to offend, or may tiptoe around a treatment session where we may have otherwise taken a more confident approach. My hope is that practitioners will leave my course Sex and Religion confident in their abilities to provide the highest level of care with confidence, sensitivity, and compassion for all of their patients.
-Rivki Chudnoff. A Case Study in Cultural Sensitivity. Friday, 14 April 2023
Application Fee: $450.00 Experience Level: Beginner Contact Hours: 15
Course Date: January 20-21, 2024, June 15-16, 2024, and October 19-20, 2024
Anatomical information centralized around the medical field has been historically male-dominated, affecting how the world discusses and understands anatomy and their bodies even in the current day. In 2005 Wade, Kremer and Brown ran a study on college students and found that 29% of women and 25% of men could not identify the clitoris on a diagram of the vulva. We need to revolutionize female sexuality in general, change the focus from the linear model where penetrative sex and orgasm are the focus as it’s been traditionally taught.
The full clitoris goes far beyond the crown which is the external tip. The clitoris actually extends several inches into the body where it branches into a shape similar to a wishbone. I want to share a description that I love from Latham Thomas, “It’s all this amazing erectile tissue that wraps around, and it all engorges when it’s stimulated. Pound for pound, if you have a vulva, you actually have the same amount of erectile tissue that people with penises have, but it’s just internal.” These clitoral legs are responsible for the sensations where the front wall of the vagina connects to the paraurethral glands (the G-spot) and for female ejaculation.
I authored the Herman & Wallace Sexual Medicine in Pelvic Rehab course for practitioners to have a platform to learn proper anatomy, identify misconceptions, and understand that sexuality is circular with satisfaction as the focus. With the understanding of ‘normal’ anatomy and function, we can help our patients with sexual dysfunctions return to a healthy sexual lifestyle.
Sexual Medicine in Pelvic Rehab is a two-day, remote continuing education course designed for pelvic rehab specialists who want to expand their knowledge, experience and treatment in sexual health and dysfunction. This course provides a thorough introduction to pelvic floor sexual function, dysfunction, and treatment interventions for the gender and sexual spectrum, as well as an evidence-based perspective on the value of physical therapy interventions for patients with chronic pelvic pain related to sexual conditions, disorders, and multiple approaches for the treatment of sexual dysfunction including understanding medical diagnosis and management.
Lecture topics include hymen myths, female squirting, G-spot, prostate gland, female and male sexual response cycles, hormone influence on sexual function, anatomy and physiology of pelvic floor muscles in sexual arousal, orgasm. Other topics include the function (and specific dysfunction) treated by physical therapy in detail including: vaginismus, dyspareunia, erectile dysfunction, hard flaccid, prostatitis, post-prostatectomy; as well as recognizing medical conditions such as persistent genital arousal disorder (PGAD), hypoactive sexual desire disorder (HSDD) and dermatological conditions such as lichen sclerosis and lichen planus. Upon completion of the course, participants will be able to confidently treat sexual dysfunction related to the pelvic floor as well as refer to medical providers as needed and instruct patients in the proper application of self-treatment and diet/lifestyle modifications.

Aparna Rajagopal, PT, MHS, WCS, PRPC, Capp-OB Certified, and Leeann Taptich DPT, SCS, MTC, CSCS co-authored the course, Breathing and the Diaphragm: Pelvic and Orthopedic Therapists, which helps clinicians understand breathing mechanics and their relationship to the pelvic floor.
Assessment of both static and dynamic posture is something we are taught very early on in physical therapy school. Posture and postural deviations have been shown in the literature to have a direct correlation to pelvic floor function and dysfunction. Multiple EMG studies have demonstrated that foot/ankle position can influence pelvic floor activity and that there is increased pelvic floor activity with the ankle positioned in dorsiflexion.(1)
Similarly, increased thoracic kyphosis and decreased lumbar lordosis can increase the likelihood of developing pelvic organ prolapse by influencing intra-abdominal pressure and causing extra pressure on the pelvic floor. Postural deviations far away from the pelvic floor can also affect the pelvic floor. Rounded shoulders and forward head posture are common findings during our assessments. Shoulder protrusion is a common finding in chronic pelvic pain patients.(1)
Education about posture during Activities of Daily Living by itself can lead to significant improvement in Pelvic floor muscle power, and endurance.(3) Understanding myofascial connections, is a small start in understanding how/why some of these things occur. The myofascial connections from the Thoracolumbar fascia connect the pelvic floor muscle to the sacrum and the neck.(2) It also connects the Gluteals, the Latissimus dorsi, and the External Obliques to the pelvic floor.(2) Optimal functioning of the pelvic floor depends on the entire chain of the musculoskeletal system. 2 Incorporating a full body assessment including the myofascial system is important in treating patients with pelvic dysfunction.
In the Breathing and the Diaphragm course taught by Aparna Rajagopal and Leeann Taptich, various commonly seen postures, thoracic mobility and how it relates to these postures, as well as all the myofascial connections to these postures will be discussed. The implementation of a regional interdependence model is discussed to ensure a holistic assessment and treatment plan. Join them on December 9 and 10, 2023 to learn more about posture, breathing, and the pelvic floor.
References:
- Zhoolideh P, Ghaderi F, Salahzadeh Z. Are There Relations Between Posture and Pelvic Floor Disorders? A Literature Review. Crescent Journal of Medical and Biological Sciences. 2017; 4(4): 153-159.
- Tim S, Mazur-Bialy AI. The Most Common Functional Disorders and Factors Affecting Female Pelvic Floor. Life. 2021; 11: 1397. https://doi.org/10.3390/life11121397.
- Jorasz K, Truszczynska-Baszak A, Dabek A. Posture correction therapy and pelvic floor muscle function assessed by sEMG with intravaginal electrode and manometry in female with urinary incontinence. Int J of Environ Res and Public Health 2023;20:369. Doi:10.3390/ijerph20010369.
Breathing and the Diaphragm
Price: $450.00 Experience Level: Beginner Contact Hours: 14 hours
Course Date: December 9-10
Description: This remote continuing education course is presented live on Zoom and is designed to expand the participant's knowledge of the diaphragm and breathing mechanics. Through multiple lectures and detailed labs, participants will learn how the diaphragm, breathing, and the abdominals can affect core and postural stability through intra-abdominal pressure changes.
As an integrated approach, the course looks at structures from the glottis and the cervical region to the pelvic floor and helps in understanding a multi-component system that works together. Optimal function of the diaphragm and breathing patterns are key to a healthy pelvic floor, a normal functioning core, and postural stability. Evidence-based methods to assess the diaphragm and breathing mechanics are presented along with easy-to-apply practical intervention strategies.
This course includes assessment and treatment of the barriers by addressing thoracic spine articulation and rib cage abnormalities in the fascial system of muscles related to breathing and the diaphragm. The assessment concepts and treatment techniques can easily be integrated into a therapist's current evaluation and intervention strategies.
The course information is applicable to patients who present with Diastasis Rectus Abdominis, pelvic pain, incontinence, prolapse, cervical/thoracic/scapular/ and lumbar pain. In addition, current literature has shown that these breath and diaphragm training techniques can effectively improve athletic performance in Labs will be demonstrated and will be participatory where possible.
Participants may practice labs on a family member or friend or team with a fellow participant where possible.

The upcoming Modalities and Pelvic Function course is a collaboration of different faculty members working to bring participants the information they have been asking for about modalities, ever since COVID forced a shift in Herman & Wallace's course format. This is a two day, in-person, hands-on course, created to be a very research based and intervention heavy learning experience for participants.
The majority of the in-person learning is interactive or lab based with the lectures being primarily focused on how to apply these modalities to clinical experiences and practice. If you can think of a modality, it is probably mentioned, if not practiced or sampled during this class. You can check out the schedule for an extensive list of all of the modalities included in this class. If there was a modality that could not be experienced as a group, there are interspersed expert interviews reviewing those concepts.
This class is for all types of learners and will definitely meet the needs of people missing in person learning opportunities. Because this class is so lab focused, hands-on and has so much equipment involved, there will only be a few offerings with small in person class sizes.
From the Desk of Holly Tanner (Director of Education)
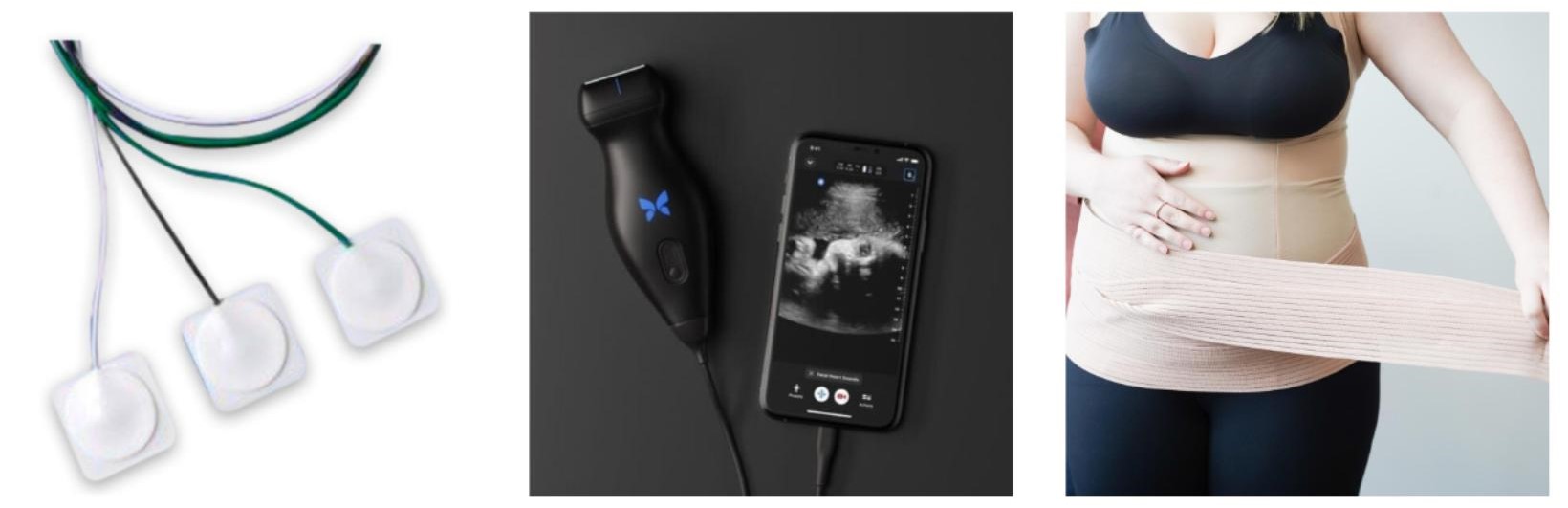
One of the course content pieces that was left out of the Zoom world transition in our popular Pelvic Floor Level 1 course that introduces participants to the world of pelvic health has been our usual modalities focus, namely that of surface electromyography (sEMG) training and electrical stimulation. For the right patient, these tools are efficient and effective; the equipment is also difficult to ship to multiple Satellite locations around the country. Herman & Wallace is thrilled to announce that not only have we solved this issue, but designed a way for clinicians to learn about dozens of modalities in an environment that allows the clinician to move beyond theoretical and soundly into the practical delivery of a variety of technologies and tools.
The new Modalities and Pelvic Function course answers the clinician’s need to understand how to choose and access the right tools both for in-clinic care and for patient self-care application. While biofeedback and electrical stimulation are covered in this course, so are introductions to understanding tools such as shockwave, dry needling, real time ultrasound, laser, and electrotherapies. With hands-on lab time, and learning modules grouped into tools specific to pelvic health conditions such as bowel dysfunction, sexual health challenges, practitioners will have the opportunity to trial a variety of tools and applications that previously may have only been available as an image in a presentation.
Current Medical Technologies will be in-person with us as we design this learning experience and will be available to answer your questions about products and clinical set-up. The interactive environment has been designed to be stimulating and allow the clinician to apply a variety of learning strategies including tactile opportunities to try things on themselves or a lab partner. This is a unique course that provides foundational understanding of technology and tools, clinical practice research and recommendations in an in-person environment. Many equipment providers have been generous in providing sample products for trial and even some giveaways to take home! We believe this modalities course is so foundational to our skillset in pelvic health that we almost put into our core pelvic function series lineup. If you’re wondering “when should I take this course?” the answer is “as soon as you can!” The only pre-requisite for this course is having taken one entry-level pelvic health course that instructs internal pelvic health examination.
Price: $645.00 Experience Level: Intermediate Contact Hours: 18.5 hours
Course Dates & Locations Coming Soon!
Now Seeking New Hosts!

Herman & Wallace is excited to announce that beginning in 2024, we will be offering our Pelvic Floor Series courses with in-person instruction.
This means that we are seeking hosts who are interested in having a faculty member come to their location to teach one of the following courses:
- Pelvic Function Level 1
- Modalities and Pelvic Function
- Pelvic Function Level 2A/2B/2C
- Dry Needling and Pelvic Health
If you are in a densely-populated area and have a space that can accommodate 36+ course participants and are interested in hosting an in-person event, please review the information at https://www.hermanwallace.com/host-a-course and let us know!
For those with slightly less space, we are actively seeking hosts for courses offered in the Satellite Lab format. Satellite lab courses use video conferencing to allow smaller groups around the country to learn under the direction of local lab assistants. If you would like to host a satellite, and have space for 16+ course participants, visit https://www.hermanwallace.com/host-a-course to get in touch.


Thank you to author Serra Shelton, SPT for sharing her article with the Pelvic Rehab Report. You can find Serra's original article published on the Empower Physiotherapy website: https://www.empower.physio/blog-all/aghx7wyg00seoe5ylk5mh3gadvr1a7. You can learn about making your practice more inclusive and comprehensive in Brianna Durand's upcoming course, Inclusive Care for Gender and Sexual Minorities, scheduled for December 2-3, 2023.
I am a 2nd year physical therapy student about to start my clinical rotations, and I have been interested in pelvic floor PT since the beginning of my academic journey. However, since it is a somewhat niche specialty, my general coursework provided only 2 lectures on pelvic floor therapy in the entire program. Despite seeking out exposure to pelvic floor education in other ways, such as taking a courses with the Herman & Wallace Institute and a pelvic health elective at the University of Washington, I wanted to learn more than the brief glimpse I had seen so far—and that is how I found myself creating an independent study course with Dr. Brianna Durand, an LGBTQIA+ pelvic floor/outpatient orthopedic physical therapist. Let me give you a sense of what this experience was like.
It was the first day of my independent study in which I would shadow Brianna as she practiced.
We started off the day with a returning patient, and Brianna began by asking for updates on her symptoms. As the patient recounted her status since her last session, Brianna typed away at her computer, asking for more details here and there.
When the patient had finished, Brianna turned away from her computer, made eye contact, and said “So to recap, since our last session you had a nasal endoscopy with negative findings, you saw an endocrinologist for the first time who ordered new tests, you had another biopsy, and you had a particularly stressful week at work.” The patient nodded emphatically. I was impressed—
I had never observed a physical therapist summarizing the patient’s words back to them. It seemed like a simple yet highly effective technique for the patient to feel fully seen and heard, and to make sure no important information had been missed.
Brianna sat back in her chair, her expression concerned, and said, “It sounds like you’ve been through an incredible amount of medical stress since our last session. No wonder you weren’t able to stick with your home dilator schedule.” The patient nodded even more, and I raised my eyebrows in surprise— we had talked about the importance of empathizing with the patient’s emotions in classes, but this was the first I had seen it in action.
“Here’s my plan for the session,” Brianna continued as she listed off the types of interventions she wanted to do that day, and why. Finally, as the icing on the cake, she added “are there any things you would like to address with today’s session?”
I was awestruck.
It was new for me to watch a physical therapist outline the exercises they planned to do with the patient prior to the session, explain the clinical reasoning behind them, and encourage the patient to contribute.
It was a beautiful way to give the patient agency over their treatment and allow them to give true consent to the session, rather than being herded from one exercise to another with little explanation, as I had been trained to do so far.
As I watched Brianna treat several more patients that day, I realized that this type of care was not isolated to the first patient, and was applied to pelvic floor and orthopedic patients alike. Every session I noticed her repeating back the patient’s subjective, validating any strong emotions the patient might be feeling, outlining the planned treatment session, and asking for input. This was simply her standard of care for everyone who walked through her door, and I was impressed by the skill and care with which she executed it.
I think Brianna delivers such consistently exceptional patient care in part because of her training in pelvic floor physical therapy.
Due to the sensitive nature of that body region, pelvic floor physical therapy faces the practitioner with some of the most vulnerable, traumatized, ashamed, and fearful aspects of the patient’s life.
From what I have seen so far, the specialty has evolved to meet the needs of its patient population by leaning into gentleness, empathy, deliberateness, and a return of agency to the patient in a way that the wider world of physical therapy could benefit from. For example, one lecture from a pelvic floor elective class I took discussed consent and trauma-informed care more thoroughly than all the rest of the two years of my program combined.
Additionally, a Herman & Wallace Pelvic Floor class I attended last spring went in-depth into exam strategies to give the patient more agency and how to build comfort for saying “no.” The instructors counseled us to use these strategies with all of our patients, whether we are aware of a trauma history or not, because every pelvic floor patient benefits from this level of thoughtful care. I would take it one step further, and argue that every physical therapy patient in any setting or specialty benefits from this type of communication and care.

I think pelvic floor physical therapy should be included more in the core curriculum of physical therapy doctorate programs.
The philosophy behind pelvic floor care would improve student’s abilities to engage with difficult patient experiences, whether they practice pelvic floor therapy after graduation or not. Experience of trauma is not limited to the pelvic region, and any instance where someone’s body is touched against their will can create a traumatic experience.
We do not know if something seemingly harmless, such as a tactile cue to the low back, could cause a patient to feel out of control of the situation or bring back traumatic memories. I have often wondered this as I watch the way our profession tosses exercises at patients, thrusting weights and straps into their hands, bundling them onto a machine before explaining what the machine does, correcting and poking and instructing with little respect for the incredible trust it takes to allow yourself to be touched by a stranger. Could we take the time to be more thoughtful about the dynamic we create with patients? Would we see better health outcomes if we did?
I first became interested in pelvic floor physical therapy before applying to graduate school, when trying to connect myself with the community of queer physical therapists in my area. Not surprisingly, many of the LGBTQIA+ therapists I networked with were also pelvic floor specialists.
Because the genital region is the site of so much social, medical, and political trauma for those of us who are sexual and/or gender minorities, I think there is a desire to provide the type of safe, sensitive medical care to our community that we have struggled to find ourselves, to be one provider not adding to the horror stories our queer friends come home with every time they visit the doctor.
I believe that because of our insertion of ourselves into this specialty, the pelvic floor world has adapted to inclusivity in ways the rest of the physical therapy field is still struggling to catch up to. If you are treating a shoulder, you can culpably ignore the lived gender experience of your patient; however, if you are examining their pelvis, you cannot so easily bury your head in the sand. The difference has been stark in my experience as a student—within the general anatomy courses of my program, professors struggled and resisted using gender-neutral anatomical terms and persisted with language such as “male anatomy” and “biologically female,” despite widespread student protest.
From the first moment of my Herman & Wallace Pelvic Floor Level 1 course I took last spring, however, the instructors all consistently used gender neutral language such as “pregnant people” and “pelvis containing a penis” without fuss or fanfare. It was enough to make me want to weep with joy, to see how possible it was to have an inclusive and non-gendered medical education. The same experience was repeated later that year, when I took a pelvic floor elective as part of my second year coursework—even though my other coursework at that institution had no policy on inclusive language, the professors of this one elective course made a point of using gender neutral anatomical language throughout.
This is another huge gift that the pelvic floor community has to offer the wider field of physical therapy—an honest look at the impact our current medical language has on LGBTQIA+ patients, and how we can shift our teaching styles to do less harm. I think if pelvic floor physical therapy were more integrated into physical therapy core curriculum, we as a profession would become better healthcare providers to LGBTQIA+ patients across every physical therapy setting.
The nine weeks I worked with Brianna was an eye-opening experience.
She demonstrated a type of patient-centered care that I hope to emulate in my own career. I was reaffirmed in my reasons for being drawn to pelvic floor physical therapy, and gained a new appreciation for what pelvic floor physical therapy skills will add to my quality of care, across all settings and all patients I treat.
I was able to have vulnerable conversations about providing the best possible healthcare to members of my LGBTQIA+ community, and discuss queer-related patient care questions with her that professors at my program do not know how to address. I appreciate that doctorate programs are already intense educational experiences with little room to add to the curriculum, but in this case I think it is crucial for pelvic floor physical therapy to become a larger part of the core curriculum. It’s not just a matter of exposing students to a potential niche specialty, it’s about integrating a style of practice that will change the culture of our field of physical therapy to one that is more patient-centered, inclusive, empathetic, and intentional.
Inclusive Care for Gender and Sexual Minorities

Price: $495.00 Experience Level: Beginner Contact Hours: 15.5 hours
Course Date: December 2-3, 2023
Description: As healthcare providers, we often want to provide compassionate, well-informed, healing care that addresses the patient in their entirety. While many have taken active steps to be more inclusive and comprehensive in their treatment, it can remain a daunting task where one is uncertain where to begin. This 2-day online course is packed full of clinically relevant and applicable information designed to help those who are striving to reframe their understanding of sex and gender.
Participants will gain up-to-date, in-depth knowledge of the various terminology used by and relating to LGBTQ+ individuals. They will also acquire an understanding of the social, economic, psychological implications on the health of this community. This course will emphasize clinical interactions, currently available research, and professional accountability.
When it feels overwhelming and nuanced, it can be tempting to avoid uncomfortable topics altogether. However, attendees for this course can expect to be gently guided into the sometimes confusing realm of gender and sexual orientation and identity. This course will provide a safe space to ask all the questions about caring for LGBTQ+ patients and practicing the skills needed to help advance your practice. Although this course will cover pelvic floor physical therapy specifically, it is appropriate and useful for any medical professional as we all have patients in the LGBTQ+ community
By accepting you will be accessing a service provided by a third-party external to https://hermanwallace.com/