Today we hear from Herman & Wallace instructor Dustienne Miller CYT, PT, MS, WCS. Dustienne instructs the Yoga for Pelvic Pain course. Join her next month at Yoga for Pelvic Pain, Cleveland, OH on July 18 and 19!

We all know yoga can help chronic headaches, insomnia, anxiety, low back pain, and a myriad of other conditions. How can we apply the principles and benefits of yoga to the treatment of chronic pelvic pain?
Breathing
As rehab professionals who treat chronic pelvic pain, we know how critical it is for our clients to learn how to downtrain the nervous system. Breath awareness and training are a useful tool in reducing sympathetic nervous system override. Some clients may not have the awareness that they are holding their breath because of pain, or even anticipation of pain. Because of the direct mechanical relationship between the diaphragm and the pelvic floor, breath holding can lead to pelvic floor muscle holding. By building awareness, which is a learned skill, the client begins to notice and eventually control non-optimal breathing patterns.
Yoga offers several types of pranayama, or breathing techniques. Integrating breath with gentle movement has proven to be highly beneficial for men and women with chronic pelvic pain. Simple belly breathing lowers heart rate, blood pressure, and anxiety levels. For more detailed instructions on two pranayama, dirgha (3 part breath) and ujjayi (ocean-sounding breath), please click here.
Grounding
Grounding techniques decrease dissociation and anxiety. Two easy postures to practice in the clinic are Seated and Standing Mountain Pose (Tadasana). When practicing Seated Tadasana, encourage your patient to feel the ischial tuberosities heavy into the chair while imagining a string lifting up the spine and through the top of the head. When practicing Standing Tadasana, offer the imagery of a magnetic pull from the soles of the feet into the earth. For more detailed instruction on Tadasana, please click here.
Being Present
Negotiating medical system can leave clients with chronic pelvic pain feeling traumatized. Sadly, the percentage of men and women who have experienced additional traumas (ie: verbal abuse, sexual abuse) are quite high. Training the mind-body-spirit connection is helpful for the client to stay in the present moment rather than think about past painful experiences or anticipate future expectations of pain. Encourage the client to move at their pace and comfort level. Teach them gentle, loving acceptance of themselves and where they are in their healing journey. Clinicians must be mindful to avoid any potential trauma triggers (ie: teaching Supta Badha Konasana, butterfly/adductor stretch, in an open gym area). An excellent book to read to enhance your understanding of the delicacy of this subject is Overcoming Trauma through Yoga by Emerson and Hopper.
Calling all Pelvic Rehab tweeters! On June 24th, there will be a tweetchat hosted by 'Living Beyond Breast Cancer' to discuss and explore the effects of breast cancer on sexual health. Topics will include:
- How diagnosis and treatment side effects can affect intimacy and sexuality
- How to communicate with your cancer care team and partner
- Tips and suggestions for managing these side effects

Now, while I think it is brilliant that we are talking about sexuality during and after cancer, the panel has no input from pelvic rehab providers! We have so much to offer women in terms of sexual rehab in an oncology setting but if our colleagues and patients don't know about us.....
So some along and join the conversation on twitter on the 24th - don't forget to use the hashtag #LBBCchat. Hope to see you there to help raise the profile of pelvic rehab in the world of oncology.
Interested in learning more about sexual rehab after gynecologic cancer? Join me in White Plains NY this August!
Today we hear more from Susannah Haarmann, PT, WCS, CLT about how pelvic rehabilitation practitioners are suited to contribute to a breast oncology patient's medical team. Susannah will be sharing more insights and treatment tools at the Rehabilitation for the Breast Cancer Patient course taking place June 27-28 in Maywood, IL.

Most pelvic rehab practitioners are incredible problem solvers and independent thinkers. We understand that often our referrals from a physician occur after a battery of tests and ineffective medical interventions. We may agree to treat a patient only to find that the diagnosis is vague and the patient often feels lost and broken. So we take out our sleuth caps, ask as many subjective questions as it takes and see where our objective examination leads us. Afterwards we paint a picture of our findings, focus the patient on what is working, tell them where we are going to start and how we are going to build one brick at a time.
The same is true for rehabilitation and breast oncology. Most physicians don’t understand how our work as therapists can complement and alleviate the side effects of mainstream medical intervention, but when the pain medication no longer works, we are there. When the range of motion no longer exists to get the patient’s arm into a cradle for breast radiation, we are there. And when the patient walks in our door, we are there, quite often for a period of time that extends well beyond after treatments cease, because the potential side effects of breast cancer, if they occur, may take years or even decades to show up. The rehab practitioner understands how to prepare the patient, without fear, for what the road ahead may look like. The purpose of this education is to empower patients to serve as their own best advocates. Pelvic practitioners and breast oncology specialists are noted for their exceptional manual skills. We are also versed to pounding the pavement educating physicians, patients and other therapists alike about who we can serve and how we can be of service. We are definitely a unique breed of therapists.
The Rehabilitation for the Breast Cancer Patient course will add to the pelvic rehab practitioner's current knowledge allowing them to become a specialist. Consider the following:
A therapist understands the biomechanics of a shoulder joint and function, but do they understand how the effects of radiation, reconstruction procedures and impairments in the lymphatic system as a side effect of cancer treatment might prevent optimal upper extremity function?
A therapist may understand peripheral neuropathy and balance training or osteoporosis and aging, however, do they understand which chemotherapeutic and hormone therapies may cause these side effects and how the prognosis may differ depending upon which medical intervention was used?
A therapist may commonly treat back pain, but do they understand how a plan of care might be altered to accommodate for a patient who experienced a TRAM flap or latissimus dorsi reconstruction?
A therapist may be able to initiate a post-operative rotator cuff strengthening program for the upper extremity, but if the patient has a history of lymphedema, how do these parameters change?
A therapist may have advanced manual therapy skills, but how might one use these skills to identify and treat lymphatic cording or set safe parameters for working around radiated tissue to restore optimal function?
These are just a few of many examples of what constitutes a specialist in the field of breast oncology and each of these questions and more will be covered in detail in the course Rehabilitation for the Breast Cancer Patient.
The American Urological Association issued new guidelines in May of this year for the diagnosis and treatment of Peyronie's. The disorder, which you can read more about at this link, often leads to a curvature in the penis that can be painful, or that can lead to impaired sexual or urinary function. While the exact mechanism leading to Peyronie's is still being researched, what is known is that plaques (sometimes calcified) may form in a deep layer of thick connective tissue called the tunica albuginea that surrounds the penis.
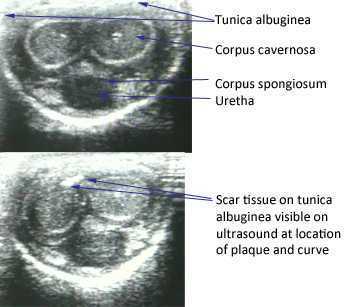
In the clinical guidelines, the authors state that a diagnostic process should include documentation of the signs and symptoms of Peyronie's disease. This can include a careful history (assessing any penile deformity, limitations in sexual function, penile pain, and level of distress). In the medical office, an intracavernosal injection (check here for a Medscape article describing an algorithm) can be completed. The authors also state, in line with expert opinion, that a provider should only evaluate a patient's Peyronie's disease when possessing "…the experience and diagnostic tools to appropriately evaluate, counsel, and treat the condition." In regards to pelvic rehabilitation, understanding the condition and encouraging the patient to visit a medical provider who is appropriately trained to manage Peyronie's is valuable. Establishing a baseline for the amount of dysfunction and curvature aids the patient and physician in determining current and future care planning.
Available treatments include education about possible treatments as well as adverse reactions to medical treatment. Interventions might include oral NSAIDs, intralesional injections (to reduce the amount of scar/thickened tissue or pain), and surgeries. Surgical options include procedures to remove the plaque or scar tissue, remodel the penile tissues after plaque removal, and for more severe cases, to implant a penile prosthesis. (Recommendations for treatments to avoid due to potential for harm or for lack of evidence are also listed in the article.)
The role of pelvic rehabilitation is emerging for men who present with genital pain, deformity, or pelvic dysfunction. There are certainly comorbid dysfunctions that we can address, such as pelvic muscle dysfunction, bowel and bladder issues if present, and we can provide a significant amount of education about pelvic health. Therapists are also teaching patients to perform connective tissue mobilization on the penile tissues, and some therapists are directing manual therapy, dry needling, and other modalities to the tissues. Rehabilitation lacks, at this time, compelling evidence to support direct treatment to the tissues, and hopefully that research will be seen in the near future. The authors of the new guidelines conclude that "…The most effective approach for a particular patient is best determined by the individual clinician and patient in the context of that patient’s history, values, and goals for treatment." This sounds to me like an effective approach for every patient who struggles with a condition that lacks a clear understanding of etiology and best treatments. These guidelines are a step forward in management of patients who deal with the frustrating condition, and the guidelines will be updated, according to the article, as the science advances.
If you would like to learn more about the rehabilitation implications of Peyronie's, and the potential and current roles of therapists in male pelvic health, you have two opportunities this year to attend the Male Pelvic Floor course , August in Denver, and November in Seattle. We expect the Seattle to course to sell out, and it's filling up fast, so check your calendar and come join us at the Male course.
Today we hear from Susannah Haarmann, the instructor for Rehabilitation for the Breast Cancer Patient. If you want to learn how to implement your pelvic rehab training with breast oncology patients, join Susannah in Maywood, IL on June 27th and 28th.

Effective pelvic rehab practitioners demonstrate many skills which are especially suitable to treat people with breast cancer, however, the first idea that comes to mind is that they understand what my friend refers to as, ‘the bikini principle.’ She remarked this week that I treat the ‘no no’ areas; the private places that we rarely share…with anyone. The reproductive regions of the pelvis and chest wall both consciously and subconsciously are associated with a plethora of personal psychological and social connotations. A pelvic health practitioner has a raised level of sensitivity to working with this patient population; there is no true protocol in this line of work, effective treatment will require a deeper level of listening and being present with the patient, and a person’s healing of the pelvic region is likely to go beyond the physiologic realm.
The biopsychosocial model of treatment is especially pertinent to the pelvic and breast oncology specialties. The breasts have great biological importance for sexual reproduction and nurturing offspring. Psychologically, breasts represent femininity for many women (and imagine how the story would change for a male with breast cancer.) Furthermore, different societies tend to create a host of rules and guidelines about what is ‘breast appropriate.’ The rehab practitioner understands that a person’s perceptions of their breasts are unlike any others and the same holds true for their cancer journey and goals with therapy.
The pelvic practitioner understands the importance of a straight face; if you have been in the field long enough something completely surprising is bound to occur, but in the day in the life of a pelvic rehab practitioner, no matter how shocking, we’ve seen it before, right? The breast oncology practitioner is going to visualize radiation burns that make their own chest wall hurt upon seeing it. Practitioners will encounter the most frustrating of severe functional deficits that could have been easily avoided had there been the opportunity for earlier intervention. The rehab practitioner providing breast oncologic care understands the story is complex, the road may be long, and although our role revolves around the body, the side effects of our treatment may have much greater reward beyond just physical function.

Today we are happy to celebrate Aline Flores, PT, PRPC! Aline is one of the newly minted Certified Pelvic Rehabilitation Practitioners, having passed the exam last month. Here's what she had to say about her career in pelvic rehab. Congratulations, Aline!
Tell us about your clinical practice
This year I opened Natura Physical Therapy, a small private practice specializing in pelvic pain and breast cancer rehabilitation. Manual therapy is a big part of our approach to patient care. I often utilize myofascial release, connective tissue manipulation, trigger point therapy, and manual lymphatic drainage during treat sessions and prescribe 2-3 specific exercises for patients to complete at home. I also provide education on the neurological/physiological/emotional response to pain and teach techniques for patients to be able to modulate this response, including breathing exercises and down training techniques. The majority of my patients are high stressed, overwhelmed and extremely hard on themselves. Helping patients become more compassionate towards themselves is a huge accomplishment.
How did you get involved in pelvic rehabilitation?
I was immediately interested in women’s health when I graduated from physical therapy school in 1997. I sought out a part time position to work/train with a therapist who was treating women with urinary incontinence. At that time I was only treating 1-2 pelvic patients a week primarily using biofeedback and muscle re-education. A year later I was hired by a hospital that was just starting a pelvic health program. Over the years I have been able to help this program grow from very basic pelvic health rehabilitation to treating much more complex pelvic health issues of like vulvodynia, pudendal neuralgia, and interstitial cystitis.
What/who inspired you to become involved in pelvic rehabilitation?
There have been so many women in pelvic rehabilitation that have inspired me and continue to inspire me. Elizabeth Nobel and Holly Herman were definitely early inspirations for me, as therapists in the founding of pelvic rehabilitation. I am always impressed the therapists who are currently making a huge impact with educating the medical community on the value of physical therapy in pelvic health issues. But, my biggest inspiration comes from my patients. Every day I learn something new from one of my patients. Whether it is a better understanding of their experience, or something that has worked, or doesn’t work for them, I am continually improving as a therapist by listening to my patients.
What patient population do you find most rewarding in treating and why?
I really enjoy working with patients with complex pelvic pain. These can be the most challenging patients to work with, but they are also the most rewarding. They keep me thinking critically. Usually these patients have a physical and an emotional component, but often have been told or assume that their symptoms are “all in their head”. It is very rewarding when I can explain the connection between the body, the nervous system and emotion, and the patient, finally feels understood. It is truly an honor to be able to work with these patients as they progress from a very difficult experience to a much more empowered state, where they have better understanding and control of their symptoms.
If you could get a message out to physical therapists about pelvic rehabilitation what would it be?
Pelvic physical therapy is much more than just “Kegels”. Issues involving bowel, bladder and sexual functioning are important activities of daily living that can have a significant musculoskeletal cause. Every physical therapist should have a basic understanding of pelvic floor muscle functioning, even if they don’t directly treat these conditions. The best pelvic rehabilitation therapists are good orthopedic therapists first.
What motivated you to earn PRPC?
Taking the PRPC exam was a challenge to myself to critically think about my knowledge base and how I practice. Although, I try to stay up to date on the most current research on a regular basis, preparing for the exam, encouraged me to be more though and consistent with my review.
What is in store for you in the future?
I hope to keep learning every day. I also plan being more involved in teaching physical therapists interested in pelvic health.

A recent study aimed to determine if an association is present between childhood functional constipation and parental child-rearing attitudes. Of the 133 studied children (ages 4-18), all were diagnosed with functional constipation and participated in a randomized, controlled trial evaluating the effectiveness of behavioral therapy compared with conventional treatment. Outcomes tools included the Amsterdam version of the Parental Attitude Research Assessment (A-PARI). The scale measures parental attitudes in the following domains: autocratic ("the child needs authority, strictness"), autonomy (encouraging independence), over-protection (prevent disappointments for the child), and self-pity (irritation with bringing up child.) (For more information about the methods, results, inclusion or exclusion criteria, you can download the linked article as full, free text.)
The study determined an association between defecation and fecal incontinence and parental child-rearing attitudes. For example, a highly overprotective or a high self-pity attitude both increased fecal incontinence, and that high autonomy and low autonomy attitudes were found to be detrimental to bowel health. The authors conclude that "…child-rearing attitudes are associated with functional constipation in children" and that parenting issues should be addressed when treating constipation in children. Specifically, if parenting issues are limiting the success of the pediatric patient or "when the parent-child relationship is at risk", referral to mental health services may be needed. The research study discusses concepts of education to "demystify" the dysfunction and positively affect parental attitudes.
We know that management of pediatric urinary dysfunction relies in large part on management of bowel dysfunction. In addition to needing to understand how we approach childhood constipation rehabilitation, we may be able to identify concerns in how a parent is dealing with a child's constipation. It is understandable that managing a child's bowel or bladder dysfunction can be frustrating for a patient, yet if the pelvic rehabilitation provider has concerns about a parent's participation in home program carryover, the parent may be appropriate for referral to a mental health provider, as this study suggests. If you would like to have more information about treating children with bowel and bladder dysfunction, you can sign up for Pediatric Incontinence and Pelvic Floor Dysfunction. You have two opportunities still this year to take this course that will prepare you for helping kids with pelvic dysfunction: Houston in July, and Boston in October
Lymphedema following breast cancer treatment, characterized by limb pain, tightness, heaviness, and possible infections, can occur during or even years following treatments for cancer. Determining which patients are at risk for lymphedema after breast cancer may allow clinicians and researchers to provide appropriate follow-up care and education. In a recent study 190 women who underwent breast cancer treatment including level 3 axillary lymph node dissection (ALND) were followed to determine risk factors for development of lymphedema. Level 3 dissection refers to the surgical classification of the axillary lymph nodes into three compartments, defined in relationship to the pectorals minor muscle. Level 3 describes the nodes above and medial to the pectoralis minor. This page includes more information about breast anatomy and the levels of dissection.
To determine the presence of lymphedema, upper limb circumferential measurements were taken. Lymphedema was found to be present in 41.5% of the women. Of these women, 44 had stage 1, 25 had stage 2, and 10 had stage 3 lymphedema. Stage 1 lymphedema is described as pitting edema that is reversible, stage 2 as non-pitting and irreversible, and stage 3 is considered advanced lymphedema with enlarged limb volume and significant skin changes. The distribution of the lymphedema was measured as 15 cm proximal to the elbow in 94.9% of the patients, and in 73.4% it was located 10 cm distal to the elbow.
In this study, the identified risk factors for developing lymphedema included axillary radiotherapy, chemotherapy, the number of metastatic lymph nodes, age and body mass index (BMI). Because of the known increase in lymphedema prevalence in patients who experience axillary lymph node dissection versus sentinel lymph node dissection, the authors recommend that physicians should play a stronger role in identifying high-risk patients and working towards lymphedema prevention. The medical prevention of lymphedema can include more frequent and thorough follow-up after surgery, and education about modifiable risk factors such as obesity. To learn more about additional lymphedema prevention educational strategies, the Institute offers Rehabilitation for the Breast Cancer Patient with instructor Susannah Haarmann. You still have time to sign up for this course that takes place at the end of the month in the Chicago area!
The following comes to us from faculty member Allison Ariail. Allison teaches several courses for the Institute, her next one being Rehabilitative Ultrasound Imaging in Baltimore, MD on June 12-14. There is still room, so sign up today!

Living in Colorado, I come across a lot of individuals who are avid runners, cyclists, or triathletes. Even with a higher level of fitness, these individuals will at times have back pain. What is going on in these physically fit, strong individuals? This is what Rostami et al.[1] set out to determine in their recent study. Using ultrasound imaging, they measured the thickness of the transversus abdominis, internal oblique, external oblique, and the cross sectional area of the multifidus while laying down as well as while mounted on a bicycle. They also measured the back strength, endurance, and flexibility of off-road cyclists with and without back pain. Fourteen professional competitive off-road cyclists with low back pain were compared to 24 control. Results showed a significantly thinner transversus abdominis, and cross sectional area of the multifidus muscle in the cyclists with back pain. There was no significant difference found in flexibility or isometric back strength between the two groups. However the cyclists with low back pain demonstrated decreased endurance in back dynamometry with 50% of their maximum isometric back strength.
The results of this study are consistent with other studies that examined less athletic individuals; thinner transverseus abdominis, and smaller multifidus muscles. This further reinforces the training of the local stabilizing muscles. What does this training method consist of? Learning to isolate each of the local stabilizing muscles; the transversus abdominis, the multifidus, and the pelvic floor muscles. Once a patient is able to isolate a contraction, challenge the muscles by holding a contraction while breathing normally, or holding the contraction while performing motor tasks such as Sahrmann’s exercises. Progress the patient so they are able to perform contractions in weight bearing positions and co-contractions of the muscles. Finally, progress the patient to maintaining co-contractions during functional activities and exercise activities. This will improve stability of the back and pelvis as well as decrease the pain experienced by the patient.
Even patients with higher levels of activity and physical fitness can benefit from a program such as this one. I have used this treatment protocol using ultrasound imaging to confirm and train the local stabilizing muscles on individuals who are both active as well as with individuals not able to participate in as much physical activity. Each and every patient has made gains, even patients who already had a higher level of activity and sports participation such as cyclists, runners, and triathletes. It is rewarding to see all patients make gains and improvements!
[1]Rostami M, Ansari M, Noormohammadpour P et al. Ultrasound assessment of trunk muscles and back flexibility, strength and endurance in off-road cyclists with and without back pain. J Back Musculoskelet Rehabil. 2014; Nov.
According to the online resource www.celiac.org celiac disease (also called celiac sprue or gluten sensitive enteropathy) is an autoimmune disorder in which the ingestion of gluten can damage the small intestine. It is further described as an autoimmune disorder affecting 1 in 100 people worldwide and a disorder that can occur among "genetically predisposed people." Common signs and symptoms include abdominal bloating and pain, chronic diarrhea, vomiting, constipation, weight loss, fatigue, irritability and behavioral issues, dental enamel defects, delayed growth, failure to thrive, and ADHD. If not treated, long-term consequences may include developing other disorders such as Type I diabetes, multiple sclerosis, dermatitis herpetiformis (itchy rash), anemia, osteoporosis, infertility, epilepsy, migraines, and intestinal cancers.

Last year, in the Journal of Family Practice, an article was published describing "Why celiac disease is so easy to miss" the authors point out that less than half of patients present with GI symptoms. An unexplained symptom, iron deficient anemia, may be a clue that a patient needs to be tested for celiac disease. Other conditions, such If a patient has a 1st degree relative with celiac disease, presents with autoimmune thyroid disease, peripheral neuropathy, recurrent migraine, chronic fatigue, osteopenia/osteoporosis, or elevated liver enzymes. (See the linked article for further considerations for testing.) Blood serum tests can help determine the presence of celiac disease, and other tests such as an intestinal biopsy or response to a gluten-free diet can be used to confirm the condition. Adherence to a gluten free diet is critical for a patient with celiac disease, and if you are currently (or have tried) eating a gluten free diet, you know how challenging that may be because gluten is in so many products including sources such as vitamins, medications, and lipsticks! If your patient has been diagnosed recently with celiac disease, referral to a nutritionist may be an excellent part of the patient's plan.
While we might imagine that a patient who has a genetic susceptibility for celiac disease would be diagnosed long before we first see them in the clinic, patients can have a "triggering event" such as a trauma, infection, or severe stress that triggers an onset of the disease. And because of the common gastrointestinal symptoms that are present, a patient with undiagnosed celiac disease may be found in our clinical practice. If you would like to learn more about how celiac disease can affect our patients, those diagnosed or undiagnosed, check out the Institute's new course on Nutrition Perspectives for the Pelvic Rehab Therapist, instructed by Megan Pribyl who earned degrees in both nutrition and exercise science. The course taking place in Seattle this weekend has a few last-minute spots for you to attend, and if you'd like to host this course, contact us at the Institute!
By accepting you will be accessing a service provided by a third-party external to https://hermanwallace.com/











































