Pelvic Muscle Rehabilitation and Men's Sexual Health
Pelvic rehabilitation therapists working with men who have sexual dysfunction may be aware of the work of Grace Dorey, who published a randomized, controlled trial about pelvic muscle strengthening for erectile dysfunction. A recent article published in the Journal of the American Physical Therapy Association confirms the conclusion of Dorey and colleagues that pelvic muscle rehabilitation is beneficial in improving erectile dysfunction.
In the study out of France by Lavosier and colleagues, 122 men with erectile dysfunction and 108 men with premature ejaculation completed twenty 30-minute sessions of pelvic muscle strengthening with active contraction and electrical stimulation. In the study, a penile cuff placed around the shaft of the penis measured intracavernous pressure, electrodes applied to the "upper face of the penis shaft" provided electrostimulation at 80 Hz to the ischiocavernosus muscles, and a vibrator device applied to the glans penis provided stimulation for erection. A large computer screen displayed contractions, and the patient was allowed to increase the level of electrotherapy stimulation to maximal sensory stimulation below pain threshold. Contractions were completed at the patient's own pace in regards to frequency and duration, but each patient did have feedback about his contraction on the computer monitor in front of him. Patients were also given an intracavernosal injection aimed to create an erection lasting 30 minutes.
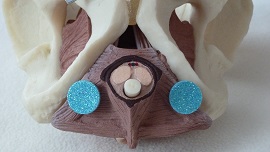
The authors describe the erection process as being both vascular and muscular, with the ischiocavernosus muscle having a significant role in erections and in ejaculation. The ischiocavernosus muscle, which is a muscle of the superficial layer in the perineum, attaches along the ischiopubic ramus and wraps around the proximal superior portion of the penis to have an effect on penile rigidity. Contractions of the ischiocavernosus appear to maintain the rigidity of the penis through compression of the roots of the corpus cavernosum, the upper portions of the penis where blood fills in the spaces.
This is a very interesting study with equipment and software created specifically for the study. Because ischiocavernosus muscle force could not be directly obtained, force variations were measured using intracavernosal pressure changes during and after pelvic muscle contractions. The authors provide a detailed description of the analysis methods as well as the challenges of measuring the ischiocavernosus muscle with other methods. The lack of uniformity in the contractions and the likelihood that all components (pharmacological, electrotherapy, vibratory stimulation, and feedback) would not be a form of therapy available to all patients in a rehabilitation setting make this study challenging to extrapolate to patient care. However, further evidence that pelvic muscle strengthening can alleviate erectile dysfunction is promising, and the study components also bring into question if patients should be utilizing vibratory therapy, performing home exercise programs for longer periods of time (up to 30 minutes), and if patients should be completing their exercises during states of penile erections. Further research will help us understand the role of each component in pelvic rehabilitation and perhaps to also learn why the results of the study were not as encouraging for premature ejaculation.
To learn more about male sexual health and pelvic floor rehabilitation, you can attend the Male Pelvic Floor Function, Dysfunction, and Treatment continuing education course, with the next opportunity scheduled in Nashville in March.
By accepting you will be accessing a service provided by a third-party external to https://hermanwallace.com/