How to Become a Pelvic Floor Therapist
 As awareness of pelvic floor dysfunction continues to grow, patients are discovering that it can be difficult to find a pelvic floor therapist who can treat them. The world needs more clinicians who can treat pelvic pain, pelvic organ prolapse, urinary incontinence, diastasis recti (mommy tummy), and the many other conditions that constitute pelvic floor/pelvic girdle dysfunction. There are several articles on PelvicRehab.com which give an overview of some of the common pelvic floor conditions in women and common pelvic floor conditions in men. Maybe you are somebody who is motivated to help these patients heal, and aren't sure where to start. This introduction is meant to help you get started as a pelvic floor therapist. You can also read some of our past interviews with featured practitioners to learn about their paths to pelvic rehabilitation on the Pelvic Rehab Report.
As awareness of pelvic floor dysfunction continues to grow, patients are discovering that it can be difficult to find a pelvic floor therapist who can treat them. The world needs more clinicians who can treat pelvic pain, pelvic organ prolapse, urinary incontinence, diastasis recti (mommy tummy), and the many other conditions that constitute pelvic floor/pelvic girdle dysfunction. There are several articles on PelvicRehab.com which give an overview of some of the common pelvic floor conditions in women and common pelvic floor conditions in men. Maybe you are somebody who is motivated to help these patients heal, and aren't sure where to start. This introduction is meant to help you get started as a pelvic floor therapist. You can also read some of our past interviews with featured practitioners to learn about their paths to pelvic rehabilitation on the Pelvic Rehab Report.
Step 1: The License to Practice Pelvic Floor Therapy
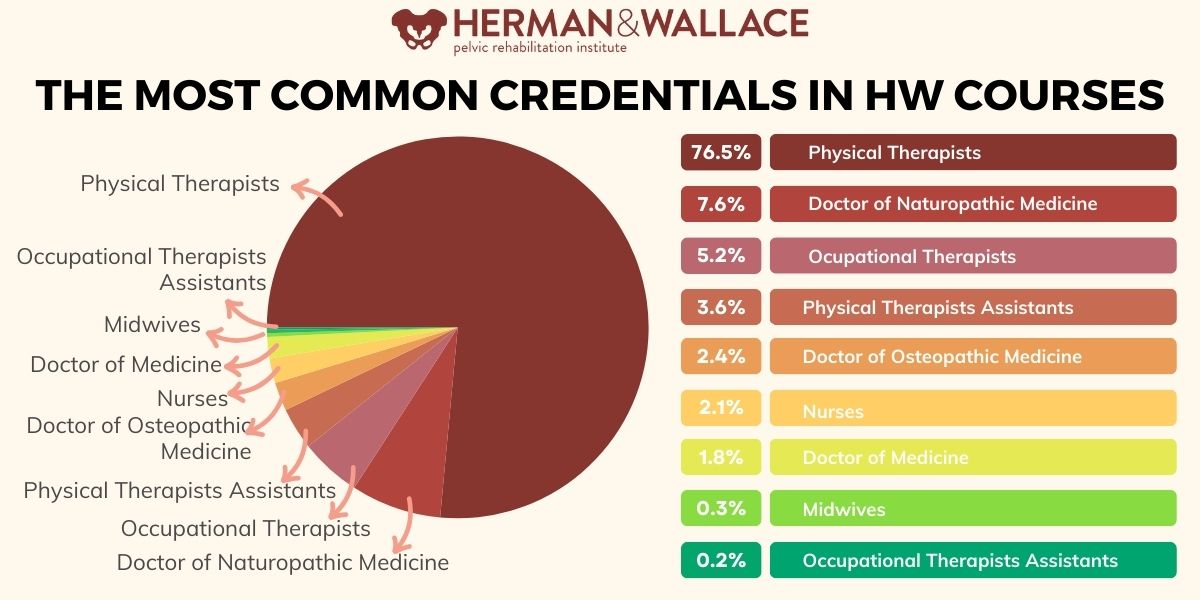
 In order to diagnose and treat pelvic floor disorders, you will first need to have an active license that enables you to conduct necessary examinations (internal and external), diagnose conditions, and prescribe treatments. If you are at the stage of deciding which license to get, be sure to consider which state you will be licensed in and look up that state's practice act, which will define any licensee's scope of practice. Currently, most clinicians who specialize in pelvic rehabilitation are Physical Therapists (PT) or Occupational Therapists (OT), though there are other licenses that will allow you to work with patients who have pelvic floor dysfunction. Many doctors, nurses, and internationally licensed medical professionals are beginning to explore pelvic rehabilitation. Over on our Frequently Asked Questions page, you can see which licenses enable a practitioner to attend a Herman & Wallace course based on their scope of practice laws.
In order to diagnose and treat pelvic floor disorders, you will first need to have an active license that enables you to conduct necessary examinations (internal and external), diagnose conditions, and prescribe treatments. If you are at the stage of deciding which license to get, be sure to consider which state you will be licensed in and look up that state's practice act, which will define any licensee's scope of practice. Currently, most clinicians who specialize in pelvic rehabilitation are Physical Therapists (PT) or Occupational Therapists (OT), though there are other licenses that will allow you to work with patients who have pelvic floor dysfunction. Many doctors, nurses, and internationally licensed medical professionals are beginning to explore pelvic rehabilitation. Over on our Frequently Asked Questions page, you can see which licenses enable a practitioner to attend a Herman & Wallace course based on their scope of practice laws.
If you are interested in becoming a Physical Therapist (PT) or Physical Therapy Assistant (PTA), the American Physical Therapy Association maintains a directory of programs that have been accredited by the Commision on Accreditation in Physical Therapy Education (CAPTE).
Is Occupational Therapy the better path for you? Here is a great blog post by faculty member and biofeedback expert Tiffany Ellsworth Lee MA, OTR, BCB-PMD, PRPC on The Occupational Therapist's Path to Pelvic Rehab.
If you have a license that is not mentioned here, please check with the agency that regulates your license to see whether pelvic rehabilitation is an option for you. Remember, your practice act must define a scope of practice which includes medical diagnosis, internal evaluations, and prescription of treatment.
Step 2: Learn to Treat Pelvic Floor Dysfunction
 Once you have a license to practice, you can start learning to specialize in pelvic rehabilitation. Many do this by taking continuing education courses, including those offered by Herman & Wallace.
Once you have a license to practice, you can start learning to specialize in pelvic rehabilitation. Many do this by taking continuing education courses, including those offered by Herman & Wallace.
Many therapists start with the Pelvic Function Level 1 course, which is designed to provide a thorough and comprehensive introduction to the anatomy and physiology of the pelvis and surrounding structures in all genders. Includes an introduction to performing intra-vaginal exams.
Pelvic rehabilitation is a rapidly evolving field and growing field. Because of this, Herman & Wallace is always updating existing courses and developing new content. Check out our full Continuing Education Course Catalog to see whether new courses catch your interest. All courses listed as “Beginner” have no prerequisites and can be taken as the first step in your continuing education journey.
Step 3: Start Practicing Pelvic Floor Therapy
 Now that you have attended a course, you have all the skills necessary to start seeing patients. Be sure to register as a trained practitioner on PelvicRehab.com so patients can find you, and maybe meet with some local referral sources to educate them about what you can offer patients.
Now that you have attended a course, you have all the skills necessary to start seeing patients. Be sure to register as a trained practitioner on PelvicRehab.com so patients can find you, and maybe meet with some local referral sources to educate them about what you can offer patients.
Senior Faculty member and Seattle clinic owner Holly Tanner, PT, DPT, MA, OCS, WCS, PRPC, LMP, BCB-PMD, CCI wrote a great blog post for the Pelvic Rehab Report about Building Relationships with Patients and Practitioners.
Looking for a new job where you can ply your trade as a pelvic floor therapist? Many employers are looking to begin a pelvic floor therapy program or expand their team, and post openings on the Herman & Wallace Job Board.
If you are starting a new clinic, you may find that you need lots of new supplies and patient resources. We are grateful to partner with several excellent providers of clinical supplies, all of whom you can find on the Herman & Wallace Course Sponsors page. We also offer many digital, downloadable products that can be used in your clinic. These products range from patient home exercise programs and intake forms to marketing supplies for your new clinic. Check them out on our Downloadable Products page.
Step 4: Continue to Develop your Knowledge and Skills
 Pelvic Function Level 1 is a thorough introductory course, and after completion, practitioners find there is so much more to learn! After each course, the therapist should begin using the skills they learned in the clinic, and choose their next course based on what patients show up. Following Pelvic Function Level 1, many may see patients with fecal incontinence or coccyx pain and may choose to prioritize Pelvic Function Level 2A (which focuses on colorectal topics) as the next step in their journey. Others who may see patients with penile pain or incontinence post-prostatectomy and may choose to take Pelvic Function Level 2C (which focuses on men's health) as their next step, or those who focus on urogynecologic conditions may take Pelvic Function Level 2B.
Pelvic Function Level 1 is a thorough introductory course, and after completion, practitioners find there is so much more to learn! After each course, the therapist should begin using the skills they learned in the clinic, and choose their next course based on what patients show up. Following Pelvic Function Level 1, many may see patients with fecal incontinence or coccyx pain and may choose to prioritize Pelvic Function Level 2A (which focuses on colorectal topics) as the next step in their journey. Others who may see patients with penile pain or incontinence post-prostatectomy and may choose to take Pelvic Function Level 2C (which focuses on men's health) as their next step, or those who focus on urogynecologic conditions may take Pelvic Function Level 2B.
Step 5: Become a Certified Pelvic Floor Therapist
 Once you have years of clinical experience, you may want to seek certification in order to distinguish yourself with a credential after your name. The certification available from HW is the Pelvic Rehabilitation Practitioner Certification (PRPC). This certification was the first of its kind and was developed to recognize expertise in pelvic rehabilitation for patients of all genders throughout the lifecycle.
Once you have years of clinical experience, you may want to seek certification in order to distinguish yourself with a credential after your name. The certification available from HW is the Pelvic Rehabilitation Practitioner Certification (PRPC). This certification was the first of its kind and was developed to recognize expertise in pelvic rehabilitation for patients of all genders throughout the lifecycle.
There are no required courses to sit for the PRPC exam. Rather, our courses instruct in the skills and knowledge one will use in the clinic, ultimately building the practical clinical experience that will be covered on the exam.
To be eligible to sit for the exam, all applicants must have completed 2000 licensed hours of direct pelvic patient care in the past 8 years, 500 of which must have been completed in the last 2 years. For more info about eligibility, please see our Pelvic Rehabilitation Practitioner Certification. page.
