Rehabilitative ultrasound imaging is a clinical tool that can change the way you practice. I have often shared with other clinicians how much the use of ultrasound imaging has influenced how I approach patients with chronic back or sacroiliac joint pain. Using ultrasound imaging allows for a way to assess the deeper core muscles, which may be more difficult to palpate on some individuals. Being able to view the activation in these muscles can inform the therapist whether the patient is properly activating their core or relying on a less ideal strategy.
Seeing the Core Muscles That Are Hard to Reach
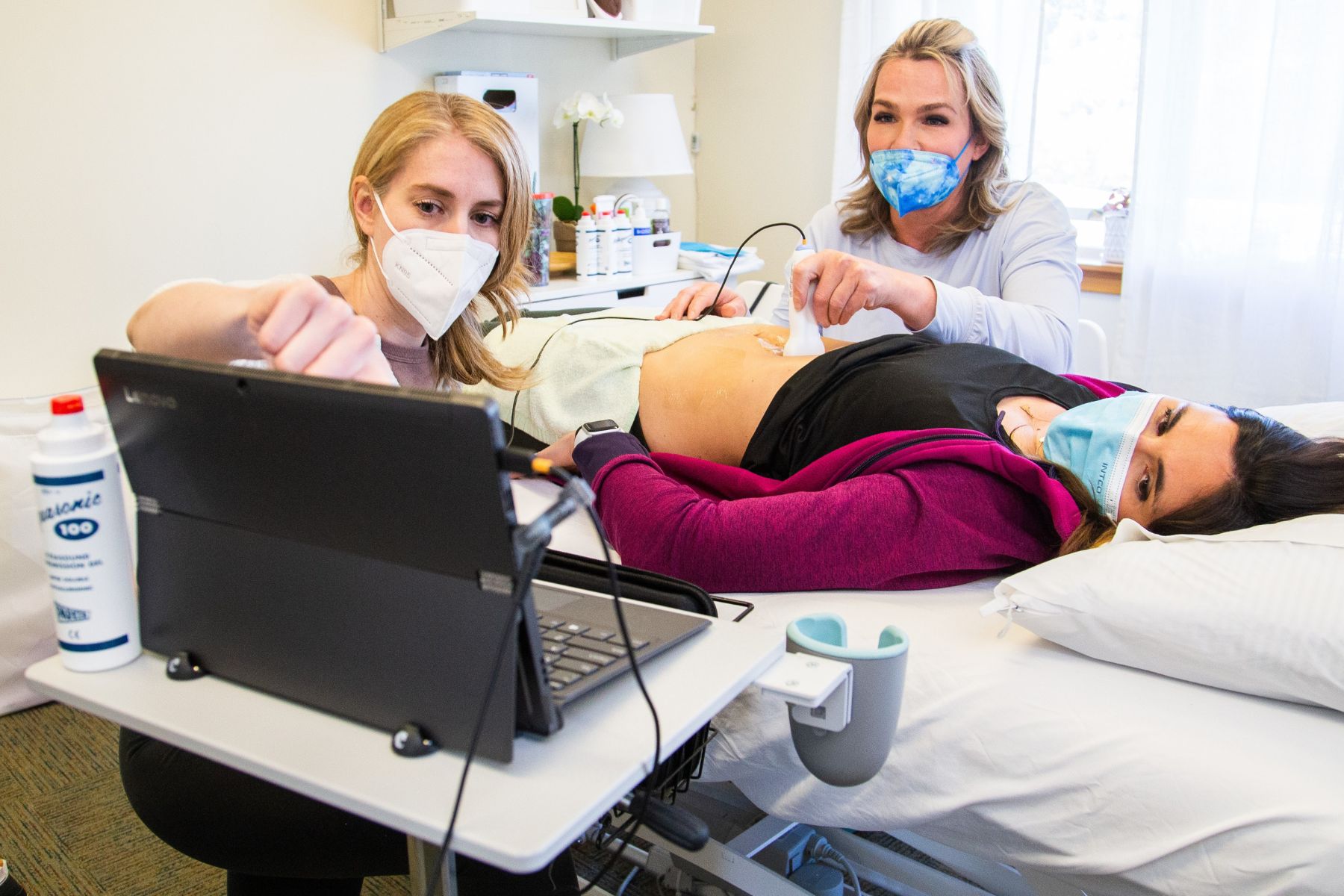
One of the most valuable things about rehabilitative ultrasound imaging in pelvic health is what it shows us about the deeper core muscles. These are muscles that conventional palpation simply cannot reach reliably in every patient. With ultrasound imaging, we can observe in real time whether a patient is using a proper activation strategy or compensating in a way that looks adequate on the surface but is not providing the stability they need.

When discussing the use of ultrasound imaging in my clinical practice, I am often asked, “What type of patient is your favorite to use ultrasound with?” This is a hard question for me to answer because ultrasound is so beneficial for several types of patients.
Ultrasound is used in a wide range of clinical scenarios, including sacroiliac joint (SIJ) and lumbar spine pain, guiding core strengthening for oncology or post-surgical patients, supporting recovery after prostatectomy, and assessing pediatric and adolescent pelvic floor function. I often highlight that ultrasound imaging is particularly valuable when internal pelvic assessments are not possible, for example, in the immediate postpartum period when pelvic rest is prescribed. In such cases, transabdominal ultrasound can help confirm whether patients are correctly engaging their pelvic floor muscles following a vaginal delivery.
A recent study in the Journal of Women’s & Pelvic Health Physical Therapy explored the use of ultrasound imaging in the early postpartum period. The study included 75 women between 0 and 5 days after vaginal delivery. Each participant took part in a single in-person session where ultrasound was used both as an assessment tool for the clinician and as biofeedback for the patient.

Have you ever gambled with what you thought was gas, only to find out that it was not? When my son was little, he asked me one day, “Mom did you ever try to fart, but it wasn’t really a fart?” At the time, I told him it was called a “shart.” Of course, being a little boy, he thought that was funny. However, being an adult and thinking you are passing gas, and it not be only gas can be mortifying. Think about how that could affect your quality of life and ability to go out in public. If you can’t trust your anal sphincters and anal canal to not know what you are letting go, it can be stressful!
What can lead to confusion and issues with sensation in this area? There are many different reasons that this area may not function ideally and be able to identify what is within the anal canal. These reasons can range from surgery in the area, radiation therapy, more minor procedures such as hemorrhoid treatment, and even chronically ignoring the urge to defecate. When sensation changes, the function of the sampling response and rectoanal inhibitory reflex (RAIR) or sampling response is changed.
The sampling response is when a small amount of fecal matter accumulates in the rectum, and a stretch occurs in the area. This then triggers a relaxation of the internal anal sphincter, and a contraction of the external anal sphincter that allows a small amount of the fecal matter to drop down into the anal canal. The contents of fecal matter are sampled, and it is determined if it is solid, liquid, or gas. If it is gas, then we can select to expel it; if it is liquid we usually respond with a stronger contraction of the external anal sphincter to hold it in. If it is solid, we can determine whether or not it is a good time to go. If it is, then we head to the restroom; if it is not, we engage the rectoanal inhibitory reflex and hold the stool until we decide there is a better time. You can see, if this sampling and identifying of the contents is off and not functioning properly, then we can have some issues arise and situations with “sharts” that would not be ideal!

Any pelvic floor rehabilitation provider knows that pregnancy can lead to changes in the pelvic floor and the abdominal wall. In the postpartum period, many individuals would like to strengthen their pelvic floor and abdominal muscles in an attempt to return to fitness and previous exercise routines. Is there a difference in how someone approaches training these muscles in the postpartum period? Will activating the muscles cause harm for our patients? This can be controversial amongst pelvic rehabilitation providers. I have heard some clinicians say that once a patient has had a pregnancy and vaginal birth, then they should never do sit-ups again, instead they should work the abdominal muscles in different ways. Others argue it depends on the individual patient.
A recent study examined the effects of different types of abdominal contractions on the positioning of the pelvic organs in nulliparous and postpartum women. Six different pelvic floor and abdominal contractions were tested, and the bladder positioning was examined using ultrasound imaging. There was significantly more lift of the bladder base when a submaximal contraction of the pelvic floor and transverse abdominis were performed with an elongation of the back. With a curl-up contraction, there was a significant amount of descent of the bladder base (Martinez-Bustelo, 2021). This increased descent of the bladder demonstrates that the choice of abdominal activation does make a difference and influences the pelvic organs. However, the overall individuality of the patient makes a difference as well. The overall management of the internal pressure system for the individual can influence the descent of the pelvic organs positively or negatively. Additionally, patients who have a diastasis recti abdominis may have additional precautions when wanting to exercise their abdomen and core.
How can clinicians observe the supportive component of the pelvic floor?
Ultrasound imaging can be performed quickly and easily, allowing the practitioner to view the pelvic organs and their response to different types of contractions. This can allow us to customize a program for post-partum individuals that are wanting to return to fitness and exercise activities and make sure that the patient is not exerting pressure into their pelvic area in a way that is not ideal. Ultrasound imaging also allows clinicians to treat postpartum patients sooner. We can treat them immediately in the postpartum period. We do not need to wait until the patient is cleared for internal work or deal with lochia for an external assessment. We are able to immediately help our post-partum patients through abdominal imaging.

When it comes to treating defecatory disorders, particularly fecal incontinence and chronic constipation, innovation can be a game changer. Enter rectal balloon catheters—a tool that, despite initial discomforting imagery, offers significant benefits for patients struggling with these conditions.
At first glance, the thought of a balloon being inserted into the anus may provoke apprehension. However, it's essential to understand that the size of these balloons is smaller than that of an average bowel movement, making their use far more manageable than one might expect. The primary role of these catheters is to provide sensory retraining in the anal canal, an aspect of treatment that is otherwise challenging to achieve.
Numerous studies have highlighted the effectiveness of rectal balloon catheters. For instance, research by Bright et al. in 2005 showed that when patients squeeze to retain a balloon, it effectively mimics the physiology of defecation. This process aids in improving maximal anal squeeze pressures, a vital aspect of bowel control.

Prostate cancer remains one of the most commonly diagnosed cancers among men, yet the pathway to effective screening can be fraught with confusion and uncertainty. With varying recommendations from different health organizations and a multitude of testing options available, patients often find themselves unsure about when and how to pursue screening. Two of the screening methods often recommended are the Prostate-Specific Antigen (PSA) test and MRI.
Prostate-Specific Antigen (PSA) Testing
Screening for prostate cancer has been confusing for some patients in terms of what is recommended. Prostate-Specific Antigen (PSA) is used by some providers, but some patients are unsure when to proceed with testing. The US Preventative Services Task CDC recommends that the use of PSA screening between in men aged 55 to 69 should be an individual choice, however, it should not be performed in men over the age of 70. Other websites recommend having a discussion for screening between individuals and their medical provider, which may include PSA testing, starting at 50, earlier if there is a risk present.
Some of the issues for screening for prostate cancer with PSA include false positives that require additional testing and biopsy, overdiagnosis, and overtreatment. The treatment for prostate cancer has a lot of side effects including urinary incontinence, erectile dysfunction, and bowel issues. This is concerning when quality of life can be greatly influenced by these side effects.

Breast cancer is the second most common cancer in women, following skin cancers. In the United States, 1 in 8 women will develop breast cancer in their lifetime.
The treatments used in breast cancer also affect the pelvic floor.
Survivors report issues with pelvic floor dysfunction including incontinence, pelvic pain, sexual dysfunction, and constipation. Up to 58% of survivors report issues with bladder urgency and incontinence. (1) Around 52% of women report sexual dysfunction six months following post-breast cancer treatment, and 19-26% continue to have sexual dysfunction five to ten years after their diagnosis. (2) When compared to individuals without breast cancer, those with breast cancer presented with significantly weaker pelvic floor muscles when measured by maximal squeeze pressure and digital examination.
Additionally, the ability to relax the pelvic floor was poorer in participants with breast cancer compared to controls. (3) These are problems that pelvic rehabilitation practitioners can assist survivors with. However, not all survivors are being referred to therapy. Barriers to individuals accessing treatment for pelvic floor dysfunction include a lack of awareness about pelvic floor dysfunction following breast cancer treatments and health care professionals “not focusing on the management of pelvic floor symptoms during cancer treatment.” (4<)

- Do you work with postpartum patients and wish you could help them recover more quickly in the postpartum time period?
Do you work with pelvic pain patients who have sacroiliac joint pain?
Do you work with patients that have a weak core?
Rehabilitative ultrasound imaging is a tool that is very helpful for the clinician to assess motor control and muscle morphology. It is also very helpful as a biofeedback tool for patients trying to improve their pelvic floor or core strength.
In an article published in 2021, researchers performed a systematic review of the efficacy of rehabilitative ultrasound imaging for improving motor control exercises compared to no feedback and other feedback methods. Studies included in the systematic review assessed the abdominal wall muscles, pelvic floor, serratus anterior, and/or lumbar multifidus. What they found was that rehabilitative ultrasound imaging was more effective than tactile and verbal biofeedback for motor control exercise performance. Patients using ultrasound imaging demonstrated increased muscle activity, muscle thickness, and target exercise success compared to tactile and verbal biofeedback. Additionally, longer retention was noted when ultrasound imaging was used. Having constant feedback by watching the monitor of the ultrasound while performing an exercise compared to feedback after performing an exercise showed superior motor learning long-term (Valera-Calero, 2021).
Using ultrasound is a marketing tool and something that will enhance your clinical offerings. Patients enjoy using this biofeedback method! When asked what they thought of the use of ultrasound, this is how a few patients responded:

Did you know that September is prostate cancer awareness month? As of 2020, prostate cancer is the most common cancer in men worldwide. Prostate cancer accounts for one in every 14 cancer diagnoses globally, and 15% of all cancers in patients born with a prostate. It ranks second in terms of cancer mortality in this population, second only to lung cancer.(1) A recent Lancet Commission on prostate cancer is projecting a significant increase in the number of new cases of prostate cancer annually. They are projecting that the number of new cases will rise from 1.4 million annually worldwide in 2020 to 2.9 million by 2040. This is due to changing age structures within the population and improved life expectancy.(1) This projected rise in prostate cancer cannot be prevented by lifestyle changes or public health interventions. Due to this projected increase in new cases, screening is a must and will be critical to better prognosis and survival for these patients. Along with a rise in prostate cancer, it is expected that other conditions such as diabetes and heart disease will mirror the projected increase in prostate cancer. It is recommended that screening and early diagnosis programs should not only focus on prostate cancer but “men’s health more broadly.”(1)
The Commission also recommended outreach programs to educate the population about prostate cancer. Social media and traditional media were both recommended to be used to reach individuals who may not be accessing medical care as frequently. This is something that we as rehabilitation clinicians can help with! As a rehabilitation clinician, we are expert educators for our patients. So much of what we do with patients is educate them about their bodies and things that can be done to assist in healing. We can take it a step further and educate them to have general health checks that would include screening for prostate cancer, among other screens such as for heart disease, and diabetes. We may also be able to reach other individuals by educating our patients to encourage their family and friends about the importance of general health screens. Many of us are also very adept at using social media to reach the community. Can we post something about Prostate Cancer Awareness Month? How easy is it to post a quick word about the expected rise in prostate cancer diagnoses and encourage patients to see their doctor for their annual health exam? Let’s all try to reach a few additional individuals this month in honor of Prostate Cancer Awareness Month! If we each are able to get a few more individuals in for screening, what impact could we make? This is something we should continue to do over the next several decades to encourage our patients to health screens! Mark your calendars every September to honor this month and educate our patients and their families!
To learn more about prostate cancer and how to treat this population, take Oncology of the Pelvic Floor Level 2A. This is an online course where you can learn specific techniques to help patients who have been diagnosed with pelvic cancers and colorectal cancers. It is offered September 7-8. Register today!
Senior faculty member Allison Ariail, PT, DPT, CLT-LANA, BCB-PMD, PRPC sat down with the Pelvic Rehab Report to talk about the role pelvic therapists play on the oncology team that will work with the patient throughout treatment and into survivorship and the impact pelvic health has on quality of life for people with cancer.
Alison is part of the HW faculty team that wrote and instructs the Oncology course series, the next course is Oncology and the Pelvic Floor Level 1 on January 27-28, 2024.








































