Steve Dischiavi holds credentials as a licensed physical therapist and a certified athletic trainer. He also has a manual therapy certification from the Ola Grimsby Institute and is board certified by the American Physical Therapy Association as a Sports Clinical Specialist (SCS).
The blog you’re about to read is targeted at clinicians just like myself. I was taught in PT school to evaluate the sacroiliac joint (SIJ) via a movement-based analysis. I even went on for a certification in manual therapy nearly 2 decades ago, and again was taught the movement-based approach. Well, as the song goes… “times they are a changin”….
How does a male sports and orthopedic physical therapist come to teach about pelvic health and wellness? I was fortunate enough to spend ten years in the NHL as the physical therapist and athletic trainer for the Florida Panthers. Ice hockey is one of the sports that has the highest incidence of groin strains among other pelvic related pathologies.1 As a clinician that was responsible for taking care of the world’s best hockey players, I was challenged to understand the interconnected relationships between the lumbopelvic-hip complex very quickly.
In the early years of my career development and the treatment of mostly males with pelvic pathologies, I leaned heavily on pelvic health professionals to help me understand an area of the body I received little training on in school and even less in my clinical care as a sports and orthopedic manual physical therapist. After years of treating hip and pelvic pathologies on my players I became more comfortable in this enigmatic area of the body. A good friend of mine was on faculty with Herman & Wallace and we frequently would communicate and compare notes. She was treating an increasing number of “sports hernias” (now termed athletic pubalgia or core muscle injury) and was relying on me to help her understand this injury and how to treat it. In turn, she helped me understand what went on in the pelvic health profession and what those therapists were trained to treat and how they went about it.
This collaboration eventually led to me joining Herman & Wallace and offering a sports and orthopedic perspective to pelvic floor consideration. I have attended Herman & Wallace’s Pelvic Floor courses to fully understand the training that a pelvic health therapist undergoes. Admittedly, I do not perform internal work because I have found a niche helping clinicians such as myself who understand that the pelvic floor is a key variable in human movement and we need to understand it at a much higher level than what we are exposed to in school, but don’t have the career trajectory of becoming an internal practitioner of the pelvic floor.





Dr. Dischiavi is a Herman & Wallace faculty member who authored and teaches Biomechanical Assessment of the Hip & Pelvis: Manual Movement Therapy and the Myofascial Sling System, available this August in Boston, MA.
STEM is an acronym for science, technology, engineering, and math. These fields are deeply intertwined and taking this approach could potentially be a way to facilitate the physical therapist’s appreciation of human movement.
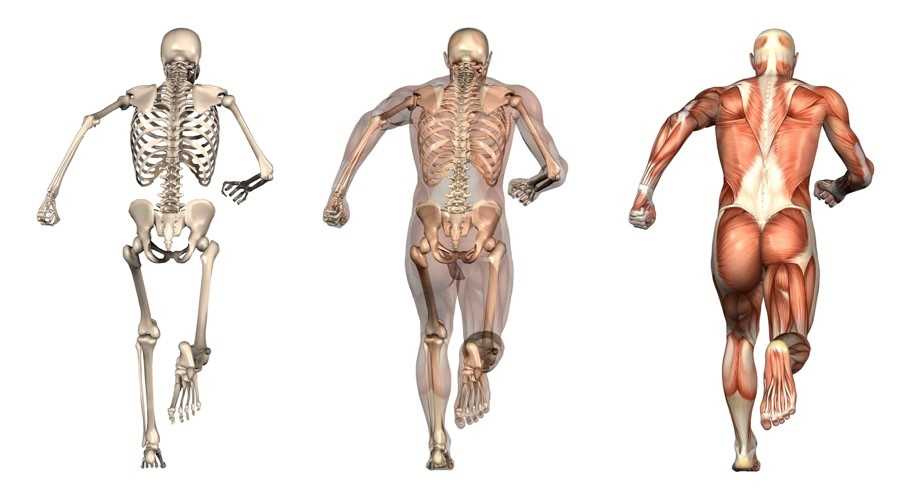
Science: I would bet most physical therapists would agree that science is the cornerstone of our profession. It is time to look across all the landscapes of science to better understand the physical principles that govern movement. Biotensegrity is a great example of how science from a field such as cellular biology can help possibly explain how we maintain an erect posture when the rigid bony structure of our skeleton is only connected from bone to bone by soft tissues [1]. The brain and central nervous system regulates muscle tone, and it is resting muscle tone that give our bodies the ability to be upright. Without resting muscle tone, we would crumple to the ground as a heap of bones within a bag of skin. Since the CNS can either up or down regulate muscle tone, this allows us to create the rigidity we need to accomplish higher level movements such as sport, and then return to a resting state after the movements are performed (see running skeleton picture below). This theory of organismic support was bred within the scientific field of cellular biology, and can potentially be applied effectively to the human organism. As physical therapists, I agree we need to be skeptical of new ideas, but we also need to embrace the idea that the physical sciences have applied to nature for centuries, and it is possible these various scientific fields can help us unlock new ideas and allow us to look at things through a different lens.
Dr. Steve Dischiavi, MPT, DPT, SCS, ATC, COMT, a Herman & Wallace faculty member, recently co-authored a peer reviewed manuscript which reviewed hip focused exercise programs. Dr. Dischiavi currently teaches a hip related course in the Herman & Wallace curriculum titled “Biomechanical Assessment of the Hip & Pelvis: Dynamic Integration of the Myofascial Sling Systems.”
"An evidence based review of hip focused neuromuscular exercise interventions to address dynamic lower extremity valgus", published in the Journal of Sports Medicine, presents evidence related to current hip focused interventions within the physical therapy profession. We know that there has been an enormous increase in the amount of hip related diagnoses and surgeries, and this calls for better knowledge from the clinicians on how to manage these particular hip related pathologies. The review finds that insufficient research has been done "to identify and understand the mechanistic relationship between optimized biomechanics during sports and hip-focused neuromuscular exercise interventions... improved strength does not always result in changes to important biomechanical variables, and improved biomechanics in sports-related tasks does not necessarily equal improved biomechanical variables in performance of the sport itself".
Biomechanical Assessment of the Hip & Pelvis is an opportunity to explore manual movement therapy with a skilled researcher and practitioner. Dr. Dischiavi has woven a very creative and innovative philosophy to help clinicians design more comprehensive hip focused therapeutic interventions. His in-depth knowledge of the evidence has allowed him to create a program that will challenge clinicians in new ways to look at the hip, pelvis, and lower extremity and how the kinetic chain can be influenced by approaching it using a new lens.
This post was written by Steven Dischiavi, MPT, DPT, ATC, COMT, CSCS, who teaches the course Biomechanical Assessment of the Hip and Pelvis. You can catch Steve teaching this course in May at Duke University in Durham, NC.
One thing that jumps out at me when treating a professional athlete, is that they have “a guy or gal” for everything! Most high profile athletes have a physical therapist, athletic trainer, acupuncturist, nutritionist, massage therapist, personal trainers for speed, power, cross fit, and pretty much “a guy or gal” for anything that has something to do with athletic performance or injury prevention. In most recent years I have been hearing more and more that athletes use someone that can analyze their movement and develop corrective exercises for them. These professionals are not just physical therapists, but some are personal trainers, exercise physiologists, chiropractors, and so on…
This post was written by H&W instructor Steve Dischiavi, MPT, DPT, ATC, COMT, CSCS. Dr. Dischiavi will be instructing the course that he wrote on "Biomechanical Assessment of the Hip and Pelvis" in Virginia this August.
In an outpatient sports medicine clinic the traditional model of physical therapy evaluation typically includes the therapist reviewing a patients chart and subjective symptom questionnaire of some sort. Then the therapist will bring the patient to an area to begin a subjective history and then onto a physical exam. After these procedures have been completed the therapist will typically assign a working clinical diagnosis and then begin treatment. In short, I would like to suggest a paradigm shift to this traditional model of thinking. Instead of starting the exam on a table with a static assessment of the structures involved and identifying the pain generator, I suggest the therapist begin with a specific set of movements used as an evaluative tool to identify movement dysfunction within the anatomical system as a whole.
All human interactions on earth occur between ground reaction force and gravity, our bodies are mostly just stuck in the middle of this constant battle and typically we succumb to whichever power exposes the weakest link in our biomechanical chains. One of the reasons the biomechanical chains in our bodies are so pliable and vulnerable to constant ground reaction force and gravity acting on them is because we are basically bones or struts suspended in a bag of skin all connected by soft tissue. Suggesting that without skin, fascia, and connective tissue supporting us, we would collapse to the ground in a pile of bones! Ingber (1997), suggested this concept, known as tensegrity, was the “architecture of life.” So in summary, the tensegrity structures are mechanically stable not because of the strength of the individual bones, but because of the way the entire human body distributes and balances mechanical stresses through the use of polyarticular muscle chains called slings. There will be more on slings in the upcoming blogs.
This August, Herman & Wallace is thrilled to be offering a brand new course, Biomechanical Assessment of the Hip and Pelvis in Tampa, FL. This two-day, orthopedic course was developed and is instructed by Steven Dischiavi, MPT, DPT, ATC, COMT, CSCS.
Pelvic Rehab Report sat down with Steve to learn more about his practice, his experience in the clinic and with the Florida Panthers hockey team and this brand new course.
What can you tell us about this continuing education course that is not mentioned in the "course description" and "objectives" that are posted online?






































