
Vestibulodynia is defined as pain at the vestibule, which is the area around the opening of the vagina (introitus). Being diagnosed with vestibulodynia can leave patients feeling frustrated because it doesn’t explain WHY they have pain at the vestibule. There are several types of vestibulodynia including infection, inflammation, neoplastic, neurologic, trauma, and hormonal deficiencies.
The most common type of vestibulodynia is caused by hormonal deficiencies known as Hormonally-Mediated Vestibulodynia. This type is caused by hormonal changes including taking birth control, breast feeding, postpartum, estrogen blockers, and peri or post menopause.
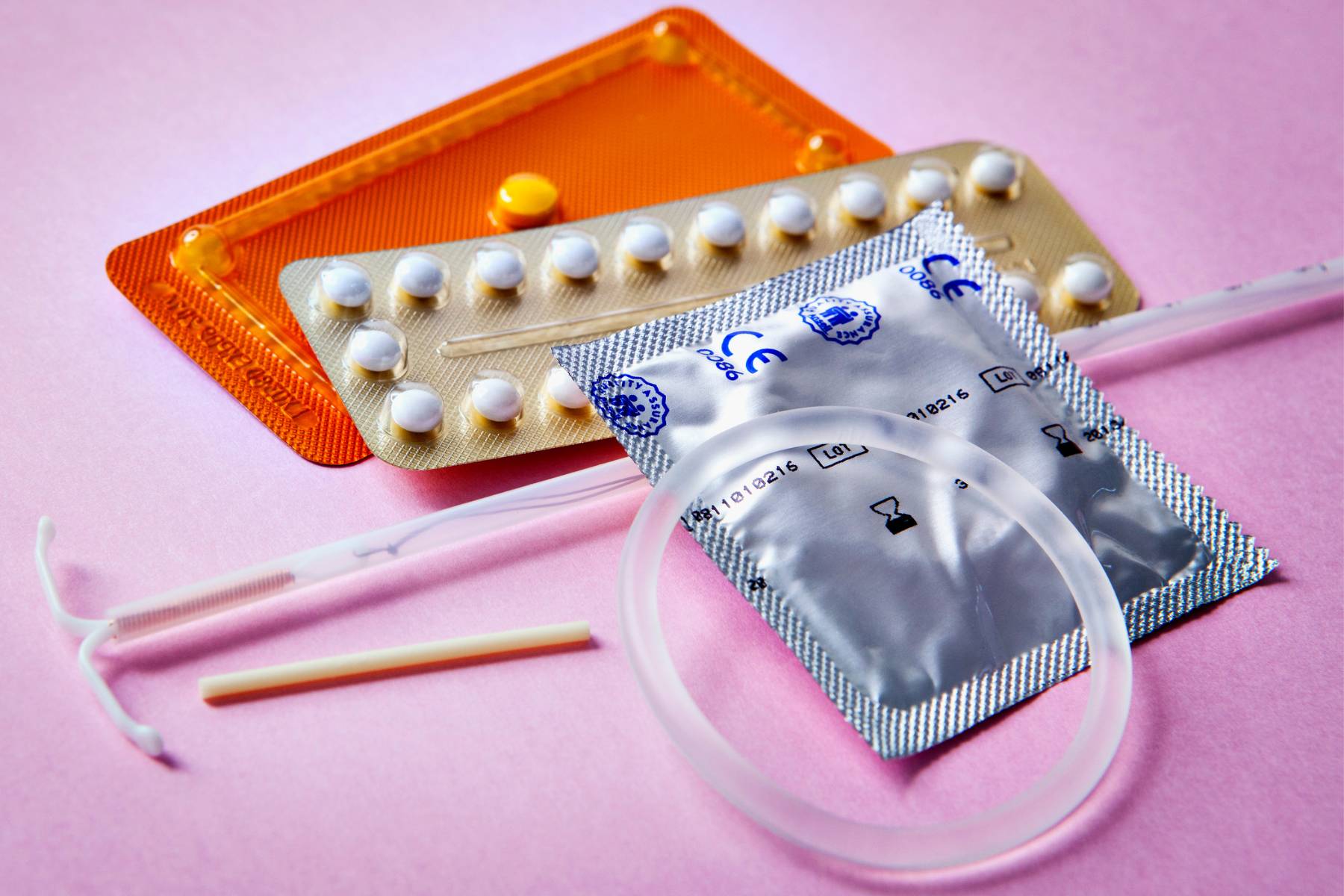
The most common cause of Hormonally-Mediated vestibulodynia in younger women (under the age of 25) is systemic birth control (i.e. oral contraceptive pills (OCPs), depo-shot, NuvaRing). Side effects of birth control (BC) such as breakthrough bleeding, nausea, headaches, increased risk of stroke, and abdominal cramping are more commonly discussed among doctors and patients.
However, what is NOT often discussed with patients prior to starting birth control, especially OCPs, is that systemic BC use causes vestibulodynia, decrease vaginal lubrication, decrease thickness of labia minora, and decreased vaginal introitus size, all leading to dyspareunia (painful sex). These changes can occur as early as 90 days after starting OCPs or with long-term use.
Unfortunately, if the onset of birth control was before the age of 17, there’s even a higher risk of developing hormonally associated vestibulodynia.1
So, WHY and HOW, does this happen?
Systemic birth control gets processed through the liver which INCREASES a protein called the Sex Hormone Binding Globulin (SHBG). SHBG binds to the free testosterone in the blood, so even if your body is making testosterone, high levels of SHBG (from the BC) DECREASE the testosterone in your body. This inhibits testosterone from getting to the tissue that needs it to be healthy—–the vestibule. The vestibule is rich with androgen receptors! If those receptors aren’t getting the testosterone (and estrogen) they need because of the increased SHBG then the vestibular tissue can become painful (vestibulodynia)!
Most commonly patients will complain about pain at the opening upon entry, dryness, friction, feeling of tearing, and actual tissue tearing resulting in bleeding, or inability to tolerate penetration at all.
Vestibulodynia can also lead to pelvic floor muscle overactivity which contributes to even more pain! Join the Sexual Medicine in Pelvic Rehab class on the weekend of June 15th-16th to learn how to identify, treat, and differentially diagnose different causes of sexual dysfunctions to get your patients better faster!
Reference:
- Goldstein, A, Burrows L, and Goldstein I. Can oral contraceptives cause vestibulodynia? J Sex Med 2010; 7: 1585-1587
AUTHOR BIO
Tara Sullivan, PT, PRPC, WCS, IF
Dr. Tara Sullivan, PT, PRPC, WCS, IF started in the healthcare field as a massage therapist practicing for over ten years, including three years of teaching massage and anatomy & physiology. During that time, she attended college at Oregon State University earning her Bachelor of Science degree in Exercise and Sport Science, and she continued to earn her Masters of Science in Human Movement and Doctorate in Physical Therapy from A.T. Still University. Dr. Tara has specialized in Pelvic Floor Dysfunction (PFD) treating bowel, bladder, sexual dysfunctions, and pelvic pain exclusively since 2012. She has earned her Pelvic Rehabilitation Practitioner Certification (PRPC) deeming her an expert in the field of pelvic rehabilitation, treating men, women, and children. Dr. Sullivan is also a board-certified clinical specialist in women’s health (WCS) through the APTA and a Fellow of the International Society for the Study of Women's Sexual Health (IF).
Dr. Tara established the pelvic health program at HonorHealth in Scottsdale and expanded the practice to 12 locations across the valley. She continues treating patients with her hands-on individualized approach, taking the time to listen and educate them, empowering them to return to a healthy and improved quality of life. Dr. Tara has developed and taught several pelvic health courses and lectures at local universities in Arizona including Northern Arizona University, Franklin Pierce University, and Midwestern University. In 2019, she joined the faculty team at Herman and Wallace teaching continuing education courses for rehab therapists and other health care providers interested in the pelvic health specialty, including a course she authored-Sexual Medicine in Pelvic Rehab, and co-author of Pain Science for the Chronic Pelvic Pain Population. Dr. Tara is very passionate about creating awareness of Pelvic Floor Dysfunction and launched her website pelvicfloorspecialist.com to continue educating the public and other healthcare professionals.
In March 2024, Dr. Tara left HonorHealth and founded her company Mind to Body Healing (M2B) to continue spreading awareness on pelvic health, mentor other healthcare providers, and incorporate sexual counseling into her pelvic floor physical therapy practice. She has partnered with Co-Owner, Dr. Kylee Austin, PT.