Many diagnoses that live under the umbrella of "chronic pelvic pain" have similar symptoms, confounding the differential diagnosis and development of a treatment pathway. Dr. Charles Butrick, in an article published in 2007, suggested that gynecologists "…be alert to…interstitial cystitis in patients who present with chronic pelvic pain typical of endometriosis." The concurrent conditions of bladder pain syndrome (BPS) and endometriosis have been described as "evil twins syndrome" in the realm of chronic pelvic pain. Bladder pain syndrome. also known as Interstitial Cystitis (IC), is a condition commonly associated with pelvic pain, bladder pressure, and urinary dysfunction such as urgency and frequency. Endometriosis can also cause or contribute to pelvic pain, and a variety of pelvic dysfunctions including bowel, bladder, or sexual dysfunction.

A study published in the International Journal of Surgery reported on the prevalence of these two conditions. Utilizing a systematic review approach, the authors located articles reporting on the prevalence of bladder pain syndrome and endometriosis in women with chronic pelvic pain. Nine observational studies were included, and the range of endometriosis diagnosis ranged from 11%-97%, with a mean prevalence of 61%. The prevalence of endometriosis ranged from 28%-93% with a mean prevalence of 70%. The large variation in these rates were explained as potentially being due to the variations in study quality and sample selection. (The authors point out that the highest rates of prevalence for BPS and endometriosis were noted in the patient groups recruited from specialist clinics and from lists of patients from operating lists.) The study concludes that in women who present with chronic pelvic pain (CPP), screening for bladder pain syndrome is important so that appropriate treatment can be directed to all issues.
If another chronic pelvic pain condition, pudendal neuralgia, is added to the diagnoses of endometriosis and painful bladder syndrome, "evil triplet syndrome" can be experienced by a patient. The various symptoms of each of these conditions can add to the total level of pain and dysfunction experienced by a woman with chronic pelvic pain. Having the tools to evaluate and treat symptomatology and address the chronic aspect of tissue, joint, neural, myofascial, and the processing of pain is a skill that most pelvic rehabilitation therapists continue to work on throughout their careers. Michelle Lyons, faculty member from Ireland, brings her "Special Topics in Women's Health" course to Chicago in a couple of weeks. Within the course, Michelle will be discussing each of these conditions from the standpoint of a multidisciplinary approach, and with the role of the pelvic rehabilitation provider in mind. She will also be sharing up-to-date and practical information about infertility and hysterectomy. If you are interested in joining Michelle and colleagues in Chicago, you still have time to sign up! And if you would like to host Michelle's course in your facility, give us a call or send us a note!
Even after teaching for a couple of decades, both in graduate level courses and in continuing education settings (live and online), I am humbled by all there is to learn and relearn about how to teach well. We all teach every day, regardless of what setting or roles we work in, and are required to share our thoughts and knowledge with respect, equanimity, and non-judgement. After teaching a course last month, I received feedback about an important topic that was not clearly addressed from an instructional or clinical standpoint, and the participant who brought it to my attention agreed to share her experience so that we as pelvic rehab providers can do a better job of addressing the issue when needed. The following post was written by Erin B. after I encouraged her to share her own thoughts about the issue.
"Having recently participated in the PF1 class after several years out of the classroom-style of continuing education, I made a few observations I felt compelled to share. (I do want to preface this with the fact that I am fully aware that my own insecurities play a role in my experiences and I recognize that they may alter my judgment of the situation.)

I am 5' 4" and currently 240 pounds. Although that is 50 pounds lighter than I was 6 months prior to attending this class, it is still significantly larger than 90% of the class participants, lab assistants and instructors. I am not someone who feels that fat is healthy. I do not feel that you need to act like I am in as good of shape as anyone else in the room. However, I do feel that there are certain assumptions made about me that are based on my physical appearance alone. Take a minute and think about your first reaction to seeing a person who is obviously overweight. (I do realize that I have made my own assumptions about some of you as well!) Just because you are much thinner and more fit looking I assume you exercise regularly, you always eat healthy and you judge me negatively for my appearance. I do know that my assumptions about you may be just as wrong as what I believe you assumed about me. However, when I see that the larger people in class have placed themselves more to the back of the room, when I have a hard time finding a lab partner and when the lab instructor struggles with how to say to the partner that got stuck with me "things may be different on her", I begin to feel like I am taking something away from the class experience for everyone else. I do not want to hinder another clinician's learning process so I don't push anyone to be my partner, but then I am actually denying myself the learning opportunities I came for. Not to mention that I may be denying the other participants the opportunity to learn how to handle a client that may look and feel like me.
The reality of our world is that there is a very large obese population. I firmly agree this leads to a multitude of chronic illnesses and astronomical medical costs for the individual and our society as a whole. It does need to be addressed on a large scale. However, we as clinicians don’t know where these individuals are on their weight journey. For someone like me who has made drastic lifestyle changes to move me in a positive direction but have not yet gotten my appearance in line with the "norm" that the health care professionals, the media and society are pushing, your response to me can be devastating to my progress, my hope and my desire to continue toward a healthier lifestyle. Again I want to acknowledge that this is as much my problem as it is for those around me and I am addressing this as well. But please have the awareness that an obese person above all is a PERSON FIRST! Then their physical size becomes just another item on the list of "facts" about them, instead of a source of anxiety and separation. Approaching an obese person with respect, acceptance, honesty and openness not only puts them at ease, it also strengthens the rapport that is so crucial in pelvic rehabilitation.
Although I was born and raised in the north east, I now live in Alabama, home of corn bread, fried chicken and sweet tea. The population I deal with is more likely to be at least overweight if not truly obese. So, quite honestly, the practical instruction of how pelvic floor evaluation and treatment may be different with the obese patient would be directly beneficial to my practice. This might include openly addressing in labs how to assess/reposition an obese patient will give each therapist an awareness and confidence when approaching this population and may minimize the patient's embarrassment and keep the doors of trust and communication open. Or taking a moment to recognize the larger participants in the classroom setting and professionally suggesting during a lab session how they can reposition themselves and still affectively achieve appropriate assessment/treatment for the patient would make the transition from class to the reality of the clinic more smooth. Also, taking a moment to offer suggestions for what the obese patient who can’t physically reach their perineum or even palpate the pubic symphysis and or coccyx and doesn’t have a willing partner to assist can do to effectively complete the rehab activities suggested. You have to admit, this is not an easy specialty of practice to broach in the first place, and anything to take the pressure off of the clinician and or patient is helpful!
I so greatly appreciate the respect and professionalism the many delicate topics related to pelvic health are addressed in this program. I would also appreciate that same respect and professionalism when it comes to the reality of the many different body types that are the represented in our practices!"
Thank you to Erin for sharing her thoughtful suggestions, and reminding instructors and fellow course participants that an open, curious and helpful approach is needed for all situations. We at the Institute will address this issue among our instructors so that we can provide more clear guidance regarding patient and provider positioning. Stay tuned for a blog post about helpful positioning and communication tips for working with patients who are obese.
Last week in our blog, you learned about Susannah Britnell, a physiotherapist who works in a multidisciplinary pelvic pain treatment setting. I learned of her clinic when I came across this journal article) about developing an interdisciplinary clinic for patients with endometriosis and pelvic pain. Below is Part 2 of the questions that she was kind enough to answer for us so that we can hear more from her perspective!

What do you find rewarding as a therapist in working in this setting?
Working with people in pain can be challenging but also extremely rewarding. I really value being able to help women realize what they can do, how they can shape their current life experience and their future. We provide tools and strategies that they can put into practice successfully. I love being able to be a part of moments when there is a shift in thinking, an opening of opportunity, when women who have seen nothing but barriers and hopelessness realize that there could be the possibility of positive change. I really find satisfaction in helping women perform daily activities, manage bladder, bowel and sexual pain concerns and increase overall activity and participation in life.
What would you say is powerful for the patients in terms of having the team available?
Patients have a great sense of support being a part of this team. Gynecological, musculoskeletal and psychosocial components are addressed with a synergistic approach. Patients are searching for answers and once they receive a diagnosis, whether its endometriosis, pelvic girdle pain, sensitization or a combination, this does help them to move forward. More often than not, the diagnosis will be a combination of gynecological, musculoskeletal, and psychosocial components, with central sensitization. When they are aware that appropriate full medical management has taken place, a readiness for change and acceptance of the active role self- management can be fostered. Our patients learn self management tools in our workshop and then we support them as they practice these and integrate them into their lives.
Our team ensures that our language and message is consistent, supportive and empowering. We work hard to avoid any language that perpetuates confusion, fear or loss of hope and we clarify any misinformation or myths patients have encountered in the past. So many women have had negative past medical experiences and feel they have not been heard, or they have been told their pain is not real. This is obviously distressing for them, so to have a team that listens, supports and then helps to give strategies for change can be a big relief.
If a concern or question comes up during a session, we can usually address this with the appropriate team member before the patient leaves the clinic. This is important as it saves time for the patient and practitioner, but also helps to resolve those unanswered questions or worries that can lead to rumination and anxiety.
Our team has weekly meetings to communicate about treatment plans, discharge planning and for problem solving particular concerns. This is invaluable for communication and helps to give our team cohesion.
What do you sense are some barriers to others creating this type of environment?
Funding would be a big barrier. The reality is that these programs cost money to run. Many of these women have experienced pain and disability for years, which of course affects all facets of life, including being able to work. They often are unable to pay for private treatment and so without a publically funded program they go without. It is challenging to decide how best to use our limited resources so that we can try to meet the needs of so many patients.
Another barrier is that there are not enough physiotherapists and counsellors that have the experience or even the interest in working with women with chronic pelvic pain, so ongoing community support and follow-up in the patient’s communities can be difficult. We have a yearly Fellowship program for gynecologists who have an interest in this area. Part of our outreach plan is to help provide educational opportunities for physicians, physiotherapists and counsellors in BC.
A common perception from the medical side is that there is no hope for these patients and that nothing can be done for them. Isolated practitioners have a high burn out rate working in the area of chronic pelvic pain. However, with a supportive team, working in this area can be rewarding and exciting.
In an ideal world, are there some disciplines that you would love to see added to this group?
It would be fabulous to have a yoga Instructor and a dietician trained in biopsychosocial approach to chronic pain.
Are there any particular patient populations or conditions you love to work with or learn about?
I love working with women with chronic pelvic pain, in particular chronic pelvic girdle pain, dyspareunia, and bladder and bowel pain.
Thank you to Susannah for sharing her knowledge and experiences in our blog! If you would like to contact Susannah she can be reached via email at sbritnell@cw.bc.ca, and her clinic website is www.womenspelvicpainendo.com. To discover more information about working with chronic female pelvic pain, you can attend one of our series courses such as Pelvic Floor Level 2B or our advanced course, Pelvic Floor Level 3. These courses always sell out, so sign up soon!
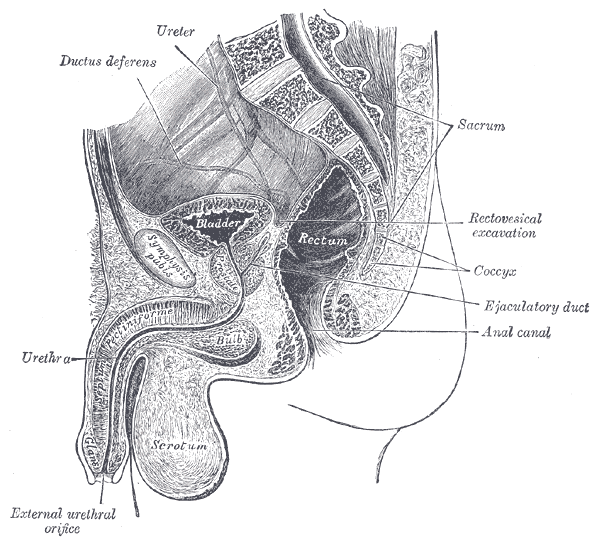
Among the challenges in research for chronic pelvic pain is the lack of consensus about diagnosis and intervention. Prominent researchers and physicians J. Curtis Nickel and Daniel Shoskes describe a methodology for classification of male chronic pelvic pain using phenotyping, which can be simply described as “a set of observable characteristics.” The authors point out in this article that men with complaints of pelvic pain have historically been treated with antibiotics, even though now it is known that most cases of “prostatitis” are not true infections. With most patients having chronic pelvic pain presenting with varied causes, symptoms, and responses to treatment, Nickel and Shoskes acknowledge that traditional medical approaches have not been successful.
In an attempt to improve classification of patients and subsequent treatment approaches, the UPOINT system was developed. The domains of the system include urinary, psychosocial, organ specific, infection, neurological/systemic conditions, and tenderness of skeletal muscles, and are listed below. Within each domain, the clinical description has been adapted from the original study (which can be accessed full text at the link above.)
UPOINT Domains
-Urinary: CPSI urinary score > 4, complaints of urinary urgency, frequency, or nocturia, flow rate , 15mL/s and/or obstructed pattern
-Psychosocial: Clinical depression, poor coping or maladaptive behavior such as catastrophizing, poor social interaction
-Organ specific: specific prostate tenderness, leukocytosis in prostatic fluid, haematospermia, extensive prostate calcification
-Infection: exclude patients with evidence of infection
-Neurological/systemic conditions: pain beyond abdomen and pelvis, IBS, fibromyalgia, CFS
-Tenderness of skeletal muscles: palpable tenderness and/or painful muscle spasm or trigger points in perineum or pelvic muscles
Within the initial research utilizing the UPOINT classification system, the authors report that most patients fall into more than one domain, and that the more domains a person is identified with, the more severe the symptoms. The domains leading to the highest impact are the psychosocial, neurological/systemic, and then the tenderness domain. The referenced article points out that the most impactful domains are the ones that are non-prostatocentric, or focused on dysfunction within the prostate itself. Phenotyping may indeed lead to improved classification of and treatment of male chronic pelvic pain. If you are interested in learning more about male chronic pelvic pain, there are still two opportunities to take the Male Pelvic Floor continuing education course this year. In August of this year, the course will take place in Denver, and in November, the male course will return to Seattle.
Grab your passports, colleagues, and head up (or down as it may be) for the 1st Pelvic Health Symposium to be offered in Toronto, Canada. The symposium will feature expert lecturers and topics that are relevant for pelvic health practitioners. The symposium is titled Beyond The Basics: Pelvic Pain and Incontinence, and topics include pudendal neuralgia, interstitial cystitis/painful bladder syndrome, vulvodynia, mindfulness, hormone therapy, and compounded medications for pelvic pain. In this one day symposium you can hear from a neurologist, urologist, gynecologist, psychiatrist, staff physician at a clinic for menopause, and a compounding pharmacist. You can access the program brochure, information about the speakers, as well as registration at the Pelvic Health Solutions website.
Pelvic Health Solutions is a practice created by Nelly Faghani and Carolyn Vandyken, two physiotherapists who are committed to providing excellent rehabilitation for pelvic dysfunctions through continuous learning, mentoring and teaching. In addition to creating practice environments that support patients with pelvic dysfunction, their website serves as an excellent resource for both clinicians and patients. Check out one of their pages here.
Because the drive to learn is so strong among pelvic health practitioners, we seem to be constantly traveling to attend workshops and increase our level of knowledge to share with our patients. Take advantage of this one-day symposium and then enjoy the beautiful and culturally diverse city of Toronto!
Bowel dysfunction is a common condition with potential for devastating limitation in a person's quality of life. Constipation, one type of bowel dysfunction, is often associated with an ability to properly coordinate the pelvic floor muscles during an attempt to empty the bowels. Instead of the pelvic floor muscles lengthening to allow the anorectal angle to increase (reducing the "bend" in the distal part of the rectum) the pelvic floor muscles might contract and thereby restrict proper emptying of the bowels. When this "opposite" or "paroxysmal" contraction occurs, a patient may be diagnosed with paroxysmal pelvic muscle function, also called dyssynergic defecation because of the lack of coordination in the muscles.
A recent study demonstrated that biofeedback therapy can be an effective tool in improving pelvic floor function for patients who demonstrate dyssynergic defecation. Magnetic resonance defecography (MR defecography) was measured prior to and after intervention, with variables of anorectal angle and perineal descent among those studied. Standard therapy was administered to 11 patients diagnosed with dyssynergia, and 11 patients received biofeedback therapy. All patients met the Rome diagnostic criteria for functional constipation, and all patients had diagnostic testing with resultant evidence of dyssynergistic muscle patterns. In addition to the MR defecography as a pre- and post-test, patients completed assessments of symptoms, quality of life, and severity of depression.
Standard therapy consisted of instructions in bowel habits, daily exercise such as walking, diaphragmatic breathing, fiber and fluid intake, defecation techniques, and timed toileting (such as attempting bowel movement 30 minutes after eating). Therapy occurred over a period of 3 months with at least once per week phone supervision. The patients in the biofeedback group were instructed in concepts of dyssynergia and in contract-relax training. Rectal sensory training with a rectal balloon was utilized if the patient had poor sensory perception. Patients were trained how to increase intrabdominal pressure while relaxing the pelvic floor muscles. They were also instructed in pelvic floor muscle strengthening, relaxation, and coordination, and were asked to complete home exercises three times per day for 10 minutes. Clinic sessions occurred at twice per week for 12 visits, then once per week for 6 visits, or a total of 18 visits over 3 months.
The authors found that paradoxical contraction and perineal descent with attempt to defecate improved significantly in the treatment group. Constipation symptoms, and depression and several quality of life scales also improved in the treatment group. Interestingly, the sense of incomplete emptying improved in both the treatment and the standard care group. While the results of the intervention are very positive, it would be interesting to include abdominal wall massage, a common technique employed to improve bowel function with constipation. If the patients demonstrated a tight pelvic floor with dyscoordinated patterns of movement, perhaps manual therapy to release tension or any pain that was present may have also been appropriate. As this is the first study to demonstrate through MR defecography an improvement in dyssynergia following biofeedback therapy, the study is very valuable to pelvic rehabilitation therapists. If you are interested in learning more about bowel dysfunction, you can start with the Pelvic Floor 2A course, which instructs bowel dysfunction including dyssynergistic defecation. The pelvic floor series courses sell out quickly, and the next opportunity to take this course is in St. Louis in October. You can also still find seats in the 2A continuing education course in the December courses taking place in Boston and in La Jolla.
We are thrilled to announce that the results of the November 2014 administration of the Pelvic Rehabilitataion Practitioner Certification (PRPC) are in! Thirteen incredible therapists have joined the ranks of Certifed Pelvic Rehabilitation Practioners!
Huge congratulations to the follwing dedicated experts who sat for and passed the exam this fall:
Lauren Calabrese, PT, DPT
Nancy Corvigno, MSPT
Rhonda Fiorello, PT, MPT
Andrea Goldberger, PT
Natalie Hickenbotham PT
Lisa Hu, PT
Rene Lawson, PT
Holly Moody, PT
Susane Mukdad, DPT
Heather Rader, PT, DPT, BCB-PMD
Elizabeth Sellhorn, PT
Reeba Varghese, DPT
Rebecca Wilcox, MPT
Check back on our list of Certified Practitioners to learn more about these therapists, as well as the other professionals who already hold this distinction.
If you are interested in learning more about certification, check out our Certification page to download the application, learn about the requirements, and access study resources. The next administration of this exam will be May 1-15, 2015.
Last week, Evidence in Motion, a large continuing education company that offers both live and online courses, announced that they are offering a new certificate program on pelvic rehab.
The Pelvic Health Certificate (PHC) includes a number of courses on male and female pelvic health.
At Herman & Wallace, we think it's wonderful to see yet another example of pelvic rehab being offered and promoted as part of "mainstream" physical therapy practice, particularly by an organization that has previously focused on orthopedics, manual therapy and sports medicine. The increased number of continuing education offerings on the topics of pelvic floor dysfuntion in men and women means that all the hard work our amazing faculty, course participants and certifed therapists have done over the years has finally brought pelvic rehab into the limelight!
Just like H&W, Evidence in Motion's program shys away from using "women's health" to stress that these courses cover pelvic dysfunction in men and women throughout the life cycle. While we are taking some issue with their contention "Sadly, once you are finished with school, you’ll be hard pressed to find a continuing education course that mentions the pelvic floor unless you find a course with “women’s health” in the title" (AHEM! Over here! Check out our incredible course offerings and our amazing and inspiring Certified Pelvic Rehabilitaton Practitioners!) we think it's wonderful to see yet another organization trying to get the word out to therapists, patients and referral sources about the incredible work our therapists do!

This fall, Herman & Wallace will be debuting a brand new course, Integrating Meditation and Neuropsych Principles to Maximize Physical Therapy Interventions, in Winfield, IL. We sat down with the course instructor, Nari Clemons, PT, to learn more about this brand new offering.
What inspired you to create this course?
There is so much more to pain management than just manual techniques, and with meditation we can help patients with a mental shift to facilitate healing. Everyone is always telling patients to work on stress management, but so few people are really able to give patients usable, practical, useful tools to do so. We all know those patients who come in so keyed up or so caught up in playing the same tape in their heads, that we are not sure what we can do to help them. I meditate every day, and it has helped my life (and my patients) beyond measure. I know how many times I use meditation as a way for patients to benefit more from their treatment. In most of the Herman Wallace courses, we talk about using down training and stress management for conditions like overactive pelvic floor, constipation, urinary urge, dyspareunia etc. (even for Interstitial cystitis, the first line of treatment is now relaxation training) but, so few practitioners have access to these tools or this knowledge, so how are they able to help patients? I want to help bridge that gap.
What can you tell us about this course not mention in the description and objectives?
This course is, above all, extremely practical. It takes away the mystery and lack of approachability of meditation, by taking the idea of centering, self-care, healing, and balancing the mind from something esoteric, vague and mystical to step-by-step tools that therapists can use. I hope attendees will use these simple techniques in their own lives and with their patients to help manage conditions of pain, tension, and anxiety. Because the aspects of health for this course border on both the realm of mental health and physical therapy, this course will be co-instructed by Dr. Shawn Sidhu, psychiatrist and meditator, who will provide info on current mental health perspectives.
Can you describe the clinical/treatment approach/techniques covered in this course?
These are all techniques that the clinician can use with the patient and the patient can use on their own. This is the piece you can give a patient to do at home. Most of these techniques can also be used as a part of treatment (ther act or neuro re-ed) to retrain muscle resting levels. I will have a CD that comes with the course that can also be used for patients at home, if the patient needs more guidance. There will be a variety of techniques, all within the realm of mind/body. Centering, observation, visualization, using mantras, affirmations, grounding, breath counting, breath control will all be addressed in a very practical and usable format.
What resources and research were used when writing this course?
I have been meditating: both learning and practicing techniques for decades, as has Shawn. I can’t tell you how many meditation and yoga workshops, books, videos and classes I have experienced over the years. I pulled heavily from that experience and my experience in the clinic and as a yoga teacher. I also bought a book that had 20 plus years of catalogued research in the fields of health and meditation to find the most clinically relevant research for PT’s. Also, I used the typical sources: pub med, medical journals. Finally, I bought all kinds of cd’s to see what was currently available. Again, I chose what I found most practical, usable (not annoying), and clinically relevant, as well as choosing a variety of styles to match different personality types/mind types.
Why should a therapist take this course? How can these skill sets benefit his/her practice?
I feel any therapist can benefit from this course because of the strength of the mind/body connection. Research has shown us that pain perception is not directly correlated with degree of injury or dysfunction. By helping your patient be in the present, rather than reacting to the past or anticipating future issues, your outcomes with your already existing manual skill set will be maximized. Similarly, as a therapist, if you can be in the present, really hear your patients, notice more with your hands, and be fully present, your interventions are certainly more directed than when you are distracted or stressed yourself. Above all, as a therapist practicing these skills, you may find yourself leading a more balanced life and less stressed by work. Certainly, not “taking our patients home with us” benefits our own health and our own families. Staying in the present moment in our own work days and our own lives ( as providers), allows us to enjoy our own lives and work days more…and who of us does not want to enjoy life more?
Want to learn more from Nari and Shawn? Join us in September for this cutting-edge course!

This post was written by H&W instructor Brandi Kirk, PT, BCB-PMD. Brandi teaches Pelvic Floor Level One and Pelvic Floor Level 2A. You can catch Brandi teaching PF2A in Maywood, IL later this month!
Recently, I was lucky enough to attend a 3-day frozen cadaver (no formaldehyde) dissection course that sparked an inquiry in my ever-inquisitive mind. While we were working on our cadaver, the coroner who was working on the other side of the complex invited us over. She wanted to show us what Crohn’s disease looks like. She had small intestines on the table and they were dissected in order to show the inside lining. The terminal ileum, where the Crohn’s disease was located, had patches of red inflamed tissue in it. The coroner proceeded to say that there was a significant amount of adhesions along the cecum, around the ileocecal valve and into the terminal ileum stemming from a prior appendectomy. Of course my mind cannot just let this information go by without some analysis…. could the appendectomy have contributed to the development of Crohn’s disease?
Travel along this thought process with me for a moment. The field of science has, to date, not found the actual cause of Crohn’s disease. With the new information I gained at my dissection course, I began to formulate a theory. My theory? Maybe the adhesions and scar tissue created by the appendectomy began to cause issues in the terminal ileum, ileocecal valve and cecum. One issue could be a decreased flow in undigested or digested food particles/chyme that causes stagnation in the terminal ileum, and over time irritation and then an inflammation of the inner mucosa. The second issue could be that the adhesions could additionally cause a decrease in circulation and lymphatic flow in the area, which also could cause an inflammatory condition.
Evidently, I’m not the only one with an inquisitive mind in the medical community! When I got home from the course, I did a search on “appendectomy and Crohn’s disease.” There is actually research that has already been completed on the topic. Some of my findings were: Appendix surgery cause Crohn’s disease? This article discusses the January 2003 issue of Journal Gastroenterology where it was found that people who had their appendix removed were 47% more likely to develop Crohn’s disease than those who did not have surgery. Badgut.org: “ IBD and Appendectomy” This article discusses the appendix having an influence over the immune system and thus appendicitis increasing the risks of Crohn’s disease. IBD and Your Appendix: This article discusses two studies on this topic. The first one showed an increase risk of Crohn’s disease within the first 20 years after an appendectomy and that women were at a higher risk than men. Unfortunately, the article did not share why the women were at higher risk than men. The second study showed a hypothesis that the original attack of appendicitis may actually be the first flare of Crohn’s disease. Potentially the patient always had Crohn’s, which went undiagnosed until the disease progressed enough. It was stated that more research is definitely needed on this correlation.
So what does this mean for practicing therapists, who are treating patients who are suffering from Crohn’s disease? If the patient has had an appendectomy, we should start there. Use all of your manual therapy skills such as visceral manipulation, myofascial release, scar massage and connective tissue manipulation in that area. In my clinical experience, which is correlated to research findings, the pelvic musculature in patients with Crohn’s disease tends to be hypertonic. These muscles need to be treated, but only after you address all of the abdominal restrictions. Through my dissection course, I was able to expand my vision about how connected the human body is. I’m afraid that as “pelvic therapists,” we tend to get tunnel-vision and we tend to blame those poor little pelvic muscles that are usually just doing their job. Yes, in the patient with Crohn’s disease they will be hypertonic, but why? They are just trying to guard and protect! They will still have to be released, but maybe not as the first step in your treatment plan. Once you release some of the fascial restrictions and improve the movement of the intestines and improve the circulation and lymphatic flow, then the pelvic muscles will not have a reason to become hypertonic again after you release them.
So let’s try to keep in mind the correlation between appendectomies and Crohn’s disease and treat those fascial restrictions first before you treat the compensatory pelvic muscles.













































