
If your experience of learning sacroiliac joint mechanics, testing, and treatment has been confusing at times, trust that you are not alone in this confusion. As students have emerged from training and coursework using a variety of models to understand the joint and surrounding structures, no wonder there is disagreement and inconsistency in clinical application of learned skills. Add to this the many names for a maneuver such as the one leg standing test, and we see that the more we can streamline updated clinical knowledge and practices, the better for our profession and for our patients. I recently enjoyed reading an article summarizing assessment and treatment of sacroiliac joint (SIJ) mechanical dysfunction by Dr. Manuel Cusi, who completed a PhD thesis regarding the joint. In the article, Dr. Cusi summarized a great deal of research-based concepts related to testing and treating this issue.
Although the structure and purpose of the sacroiliac joint are described as "controversial", the author points out the foundational concept that too much or too little stability within the SIJ can create dysfunction. The "self-bracing" mechanism is provided in the pelvic girdle via both form and force closure, and Dr. Cusi points out that this joint stability that is the aim of the self-bracing mechanism must be responsive to each specific loading condition, as a function of gravity, and with coordination of muscle and ligament forces. Also according to the article, in order to assess the SIJ, the focus must be on function rather than solely on anatomic pathology.
Mechanical testing is described as being generally divided into pain provocation or palpation tests. Although we can say, based on the literature, that no one SIJ test can provide reliable data, a cluster of several tests that are positive can provide meaningful information towards a diagnosis. In order to test various aspects of SIJ function, the following tests are listed in the paradigm model. A working knowledge of the tests below, as well as pelvic joint stability tests should comprise the clinician's "toolbox" of tests for the sacroiliac joint, and this is in addition to skills used for determining other causes of SIJ pain such as disease processes or referred symptoms.
•Posterior pelvic pain provocation test (or thigh thrust)
•Long dorsal sacral ligament palpation
•Trendelenburg test
•Stork test (or Gillet test)
•Active straight leg raise (ASLR)
•Patrick's FABER and Gaenslen's test
In relation to treatment approaches, exercise training is recommended as being divided into three stages: isolation (recruiting targeted muscle in isolation of other groups), combination (muscles are recruited in various combinations to develop endurance), and function (utilizing good technique once progressed to meaningful functional tasks). While this flow of exercise training may appear very logical, the author offers that failure to progress through these three phases may be due to several factors such as poorly designed exercises that lack specificity, progressing through exercises before patient has sufficient endurance, poor adherence, and lack of appropriate exercise technique. These factors are described in the article as intrinsic to the exercise program, whereas an extrinsic factor may be failure of the exercise program to work well because of poor ligamentous stability. In this case, the author further describes the therapeutic option of prolotherapy, which will be discussed in an upcoming post.
If you are interested in learning more about the above special tests or about treatment progressions based on technique and integration, check out Peter Philip's Sacroiliac Joint and Pelvic Ring Evaluation & Treatment. The next opportunity to take the course is in January in Seattle.

Scapular winging, also known as scapula alata (SA), describes the lack of proper muscular support that keeps the medial scapula positioned snugly against the thoracic wall. Potential causes of this condition include weakness of the serratus anterior, trapezius, and rhomboids, often related to nerve injuries of the long thoracic, spinal accessory, or the dorsal scapular nerve. Breast cancer and axillary surgery is a known risk factor for scapular winging, and the aim of a recent article was to identify patients who were at increased risk of developing the condition following radiotherapy.
Adriaenssens and colleagues report an incidence rate of scapular alata in the literature of 0-74.7%, a variability that does not help to deduce patients who are truly at risk. Women age 18 or older with a diagnosis of primary breast cancer removed by mastectomy or by breast-conserving surgery were included in their study. The pathological stage, treatment doses for radiotherapy and when applicable, the treatment doses for chemotherapy are described for the control and for the intervention group. The original study from which the data was collected is known as the TomoBreast clinical trial and focused on pulmonary and cardiac toxicity measurement. Within the data collection, scapular position was measured in physiotherapy prior to and 1-3 months following radiotherapy. (Check this link to learn more about radiotherapy.)
The physical examination included assessment of clinical symptoms like dysesthesia, heaviness, swelling, fatigue, warmth, burning, and pain. Measures of bilateral arm volume, shoulder range of motion, and the scapular slide test to assess the distance between the inferior angle of the scapula and the spine were completed. In standing, the scapula was observed for relaxed position and for scapular plane elevation to shoulder height; scapular alata was designated as present if inferior angle tilting or winging was noted.
Resulting analysis of the 119 eligible female patients include the following: prior to radiotherapy but after surgery, 10.9% (13 subjects) were positive for scapular winging. 1 to 3 months after completion of radiotherapy, winging resolved in 8 of the 13, and persisted in the remaining 5 subjects. New onset of scapular alata occurred in 1 subject. Significant factors for SA included young age, lower body mass index, and axillary dissection. Regarding the inverse relationship of increased weight to decreased scapular winging, the authors posit that patients with decreased body weight have less fat to cushion the nerves and therefore are at higher risk of nerve injury, OR that patients with higher body mass may not have winging as easily observed due to overlying adipose tissue. Having axillary lymph node dissection was confirmed in this study as a risk factor for scapular winging.
The authors conclude that scapular winging should be "actively evaluated" and describe assessments at various points in the treatment of breast cancer such as prior to surgery, following surgery, and prior to or following radiotherapy. As scapular winging correlated to loss of shoulder motion, quality of life may be impaired. If you are wanting to learn more about rehabilitation management of patients following breast cancer diagnosis and treatment, sign up now for faculty member Susannah Haarmann's Breast Oncology course in San Diego in 2 weeks! This is the last chance to take the course this year!
The Vulvar Pain Functional Questionnaire (V-Q) is provided to help patients quantify the extent that pelvic pain is affecting their lives and helps the practitioner devise a treatment strategy based on the patient's account of her symptoms.
To score the VQ: add numerical values assigned to each response. These appear next to the check-boxes. The higher the score the greater the functional limitation. A diminishing score represents improvement.
This questionnaire was developed by Kathe Wallace, PT, BCB-PMD , Hollis Herman, DPT, PT, OCS, BCB-PMD and Kathie Hummel-Berry, PT, PhD and is free to download here.
Recently, the Institute was made aware of an internet scam that is targeting physical therapists, including members of our teaching faculty. A bogus website called ComplaintsBoard has listed many PTs, including several respected Herman & Wallace faculty members, on a list of convicted sexual abusers. This site contains a similar list of doctors and lawyers that it claims have criminal records, meaning that patients or clients seeking professionals may find false and damning histories on internet search engines. The site then invites those whose names are posted to pay money through a different website to clear their records.
Clearly, this is the work of scam artists that are tarnishing the reputations of physical therapists. It is unclear who these perpetrators are, but they have targeted a number of respected professionals, including members of our faculty. Herman & Wallace is dismayed to see the character of professionals with whom we work and respect being attacked for profit. The APTA has been made aware of this, and is seeking legal action. If you find your name on such a list, please contact the APTA.
The Institute would like to make our community aware of this problem and to show our support of our faculty and our colleagues.
Please understand that, because we do not want to increase the web traffic to these scam sites, thereby increasing their efficacy, we will not be posting direct links to these sites.
A colleague recently sent an inquiry through the Institute asking if there is new research supporting pelvic floor muscle training after radical prostatectomy. As a matter of fact, I chose not to report on some recent research that I read, because it does not support conservative care for urinary incontinence (UI). The Cochrane review for postprostatectomy UI was updated this year, and the results of the review indicate that we need more and better research. (If you are unfamiliar with the Cochrane library, one of its 6 databases contains systematic reviews of the literature that are updated periodically.) Although within the abstract of the reviewthe report states that there is a lack of consistency in the interventions, the populations, and in the outcome measures, the value of conservative approaches is deemed "uncertain." The authors do conclude that benefit from one-to-one pelvic floor muscle training is "unlikely" following transurethral resection of the prostate, or TURP.
The critiques of the research listed in the review include the above mentioned lack of consistency in outcomes and interventions. Most of the studies also did not include a report of pre-surgical outcome status, of adverse effects, and lifestyle changes as an intervention was never identified in any of the research. This leads us to this question: why are we treating men for UI or erectile dysfunction (ED) if this systematic review brings into question the efficacy of what we do? Certainly patients are improving as a result of pelvic rehabilitation, or I doubt that the medical providers would continue to refer patients to the offices who provide rehabilitation to these patients. What we do not know about each of the studies is how much of the male anatomy was affected by the procedure for the prostate. The patient's pre-surgical status and the skill level of the surgeon are both known factors for outcomes following prostatectomy, yet how are those quantified in the literature?
Most importantly, how can we be a part of the solution when it comes to creating research to support the services that we provide. It may be helpful as therapists to be certain that we are maximizing the level of knowledge about the surgeries, the anatomy involved, and about the available treatments. This can mean attending coursework that is specific to or includes discussion of male pelvic floor issues. (Check out the Pelvic Floor Series level 2A course or the Male Pelvic Floor Courses offered by the Institute, especially if more male patients are finding their way to your door.) Speak with referring physicians about surgical techniques, observe some surgeries, or attend a urology conference (maybe there's one near your hometown, or you want to attend with your local referring urology group.) Always document using outcomes studies when you can. Write a case study. You can even purchase a text book that teaches you step-by-step how to write a case study. I know that you don't have time...so, create a weekly lunch meeting at work with a colleague where you each work on and critique each other's project. Getting involved with local university programs can also allow you to be part of the research solution.
In summary, we need more and better research that documents how we are helping our patients. In relation to male patients following prostate procedures, who is screening these men to decide if they have tight, painful pelvic floor muscles versus weak muscles with lack of awareness of their use? We are the best chance the patient has in helping with the rehabilitation process. It is also imperative that we are testing muscle function in men to help categorize the patient as someone who might improve with an exercise-based approach or as someone who might need a trial of pelvic floor muscle electrical stimulation. If you tend to complete internal muscle testing with women, yet feel uncomfortable with this approach in men, I encourage you to move forward in your practice of this critical skill. We need to catch the patients early on who seem to have no muscle function and no awareness, and then refer that patient back to the surgeon within a reasonable time frame if there is a lack of progress. A few of the men I worked with who went on to have a male sling had very positive outcomes, and they also were very grateful that they had a pelvic rehabilitation provider to give guidance and feedback along the way. Patients who are more aware of their pelvic muscles, how to use them (and not use them!), and who know how to take care of their pelvic muscles throughout their lifespan are better poised to handle the post-surgical pathway if they should require further intervention.
Today, September 28th, marks the ten year anniversary of the founding of Herman & Wallace! The Institute was founded on this day in 2005 by Holly Herman, PT, DPT, MS, OCS, WCS, BCB-PMD, PRPC and Kathe Wallace, PT, BCB-PMD with a mission of providing the very best evidence-based continuing education related to pelvic floor and pelvic girdle dysfunction in men and women throughout the life cycle.
![By Joey Gannon from Pittsburgh, PA (Candles) [CC BY-SA 2.0 (http://creativecommons.org/licenses/by-sa/2.0)], via Wikimedia Commons](https://upload.wikimedia.org/wikipedia/commons/thumb/f/f5/Blue_candles_on_birthday_cake.jpg/512px-Blue_candles_on_birthday_cake.jpg) Since our founding, it’s been our privilege to spread this mission through an ever-increasing number of course offerings, products, resources and certification so that therapists can meet their goals and patients can access trained practitioners who can address their needs.
Since our founding, it’s been our privilege to spread this mission through an ever-increasing number of course offerings, products, resources and certification so that therapists can meet their goals and patients can access trained practitioners who can address their needs.
In the past ten years, we’ve significantly expanded our course offerings. Currently-offered courses cover pediatrics and geriatrics, sexual health, yoga and Pilates, oncology, meditation and mindfulness, and a number of other topics instructed by some of the foremost experts in the field, with whom we are thrilled to work and provide a platform to spread their knowledge. In addition to our flagship Pelvic Floor series courses which were the first offered by the Institute, H&W now offers 46 live courses and 14 online courses on topics related to pelvic floor dysfunction, as well as related women’s health, men’s health and orthopedic topics.
We have also had the opportunity to take this mission abroad and have offered pelvic floor courses in Saudi Arabia, United Arab Emirates, Chile, Brazil, the UK and Europe. In 2013, H&W launched the first-ever certification recognizing expertise in treating pelvic floor dysfunction in men and women throughout the life cycle, the Pelvic Rehabilitation Practitioner Certification. Since then, 84 practitioners have sat for and passed this exam and earned PRPC as a designation of their competence in evaluating and treating pelvic rehab patients. This coming year and beyond, we are looking forward to continuing with our mission of providing the very best education and resources for pelvic rehab therapists. We are continuing to expand our offerings of intermediate and advanced- level Pelvic Floor coursework for experienced therapists, as well as an increasing number of scheduled events for our introductory courses so that more practitioners can begin learning the skills needed to serve this growing patient population.
Over these years, the best part is hearing from therapists that our mission is changing lives for practitioners and for patients. This recent email we received from a course participant is the best birthday gift we received!:
“I always gain so much from your courses and they are the first ones I look to each year for simply excellent use of my education dollars and to further my knowledge of Women’s/Men’s/Children’s Pelvic Health. Kuddo’s to you, sincerely, for really making a difference in the lives of so many – that you, as therapists, work with directly, AND that you “work with” through each therapist that you train. What a huge ripple effect for making the difference in the lives of many…..and on such personal issues. And I give due credit to you with each patient I see for the training I have and am still receiving! Thank-you!!!!”
 The Herman & Wallace Pelvic Rehabilitation Institute was founded nearly a decade ago by physical therapists and educators Kathe Wallace and Holly Herman. The Institute has served as a platform for foundational to advanced pelvic rehabilitation coursework that covers a wide variety of topics. Included in some of the newer coursework is content directed at more general orthopedics or women’s health topics, such as:
The Herman & Wallace Pelvic Rehabilitation Institute was founded nearly a decade ago by physical therapists and educators Kathe Wallace and Holly Herman. The Institute has served as a platform for foundational to advanced pelvic rehabilitation coursework that covers a wide variety of topics. Included in some of the newer coursework is content directed at more general orthopedics or women’s health topics, such as:
- Biomechanical Assessment of the Hip and Pelvis
- Rehabilitative Ultrasound Imaging: Orthopedic Topics
- Physical Therapy for the Breast Oncology Patient
- Neck Pain, Headaches, Dizziness, and Vertigo
- Manual Therapy for the Lumbo-Pelvic-Hip Complex.
Occasionally, as we have continued to expand our offerings at the Institute, participants have expressed concern that a few of the courses are “not pelvic floor” related. We wanted to take a moment to share our perspective regarding that concern:
1. Most pelvic rehabilitation providers are not exclusively working with patients who have pelvic floor dysfunction.
When we completed a survey of job task analysis among pelvic rehabilitation therapists, we learned that many therapists are not working with patients who have pelvic dysfunction 100% of their time, and that general musculoskeletal care makes up a large part of many pelvic rehab therapists’ caseload. Unfortunately, many patients aren’t often dealing with only one dysfunction, so our patients who present with urinary incontinence may also have foot pain, or headaches, for example.
2. Many pelvic rehabilitation providers also describe themselves as orthopedic therapists.
The majority of therapists who responded to our job analysis survey (and those who attend our courses) work in either an outpatient facility or a hospital-based outpatient facility. In fact, many of the respondents are board-certified in orthopedics. Outpatient facilities typically require that a therapist can work with any part of the body, in addition to the pelvis.
3. General orthopedic rehabilitation is closely related to pelvic rehabilitation.
There are an overwhelming number of ways that a patient’s comorbid conditions can be related to the pelvic floor. For example, a patient with foot pain may unload the involved side, placing increased strain on the hip, pelvis, and low back on the opposite side. Another patient who has poor balance may decrease their degrees of freedom by holding the trunk and pelvic muscles tense in order to compensate for a balance difficulty. A patient who has migraines may have to spend a significant amount of time lying flat when she has migraines, potentially leading to discomfort in other joints.
4. We have not decreased the amount of pelvic courses we offer in exchange for general, orthopedic courses. On the contrary, the Institute has continued to add more focused pelvic rehabilitation courses such as Post-Prostatectomy Patient Rehabilitation, Assessing and Treating Women with Vulvodynia, and Geriatric Pelvic Floor Rehab.
In short, we have chosen to offer some coursework that is not solely focused on the pelvis, because these courses can provide benefits to the therapists and to the patients they serve. The Institute is always interested in participant feedback, and is willing to try out new courses to gauge interest level and satisfaction with new courses. As always, you will be provided with the best in pelvic rehabilitation education, and have opportunities to take courses from instructors who offer additional skills and expertise. If you have any questions, or suggestions about course content, please let us know by filling out the Contact Us form on the website. And if you have an idea for a new course you’d like to teach that adds to our existing offerings, we’d love to hear from you- please fill out this form if you have a new course idea.
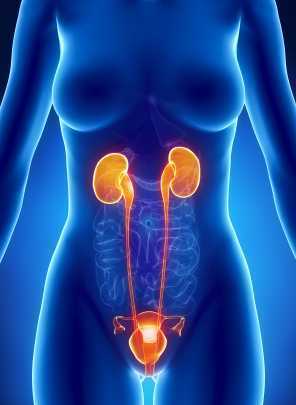
Patients who suffer severe bladder damage or bladder disease such as invasive cancer may have the entire bladder removed in a cystectomy procedure. Once the bladder is removed, a surgeon can use a portion of the patient's ileum (the final part of the small intestines) or other part of the intestine to create a pouch or reservoir to hold urine. This procedure can be done using an open surgical approach or a laparoscopic approach. Once this new pouch is attached to the ureters and to the urethra, the "new bladder" can fill and stretch to accommodate the urine. As the neobladder cannot contract, a person will use abdominal muscle contractions along with pelvic floor relaxation to empty. If a person cannot empty the bladder adequately, a catheter may need to be utilized. (A prior blog post reported on potential complications of and resources for learning about neobladder surgery.)
During the recovery from surgery, patients will wear a catheter for a few weeks while the tissues heal. Once the catheter has been removed, patients may be instructed to urinate every 2 hours, both during the day and at night. Because patients will not have the same neurological supply to alert them of bladder filling, it will be necessary to void on a timed schedule. The time between voids can be lengthened to every 3-4 hours. Night time emptying may still occur up to two times/evening. Patient recommendations following the procedure may include that patients drink plenty of fluids, eat a healthy diet, and gradually return to normal activities. Adequate fluid is important in helping to flush mucous that is in the urine. This mucous is caused by the bowel tissue used to create the neobladder, and will reduce over time.
Urinary leakage is more common at night in patients who have had the procedure, and this often improves over a period of time, even a year or two after the surgery. As pelvic rehabilitation providers, we may be offering education about healthy diet and fluid intake, pelvic and abdominal muscle health and coordination, function retraining and instruction in return to activities. In addition to having gone through a major surgical procedure, patients may also have experienced a period of radiation, other treatments, or debility that may limit their activity levels. The Pelvic Rehabilitation Institute is pleased to offer courses by faculty member Michelle Lyons in Oncology and the Pelvic Floor, Part A: Female Reproductive and Gynecologic Cancers, and Part B: Male Reproductive, Bladder, and Colorectal Cancers. If you would like to explore pelvic rehabilitation in relation to oncology issues, there is still time to register for the Part A course taking place in Torrance, California in May! If you would like to host either of these courses at your facility, let us know!
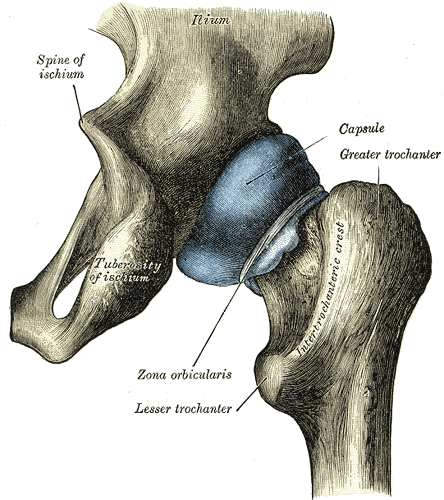
An article appearing this year in Arthroscopy details a systematic review completed to determine if asymptomatic individuals show evidence on imaging of femoroacetabular impingement, or FAI. Cam, pincer, and combined lesions were included in the results. To read some basics about femoroacetabular injury, click here. Over 2100 hips (57% men, 43% women) with a mean age of 25 were studied. (Only seven of the 26 studies reported on labral tears.) The researchers found the following prevalence in this asymptomatic population:
Cam lesion: 37% (55% in athletes versus 23% in general population)
Pincer lesion: 67%
Labral tears: 68%
Mean lateral and anterior center edge angles: 30-31 degrees
The authors conclude that femoroacetabular impingement tissue changes and hip labral injury are common findings in asymptomatic patients, therefore, clinicians must determine the relevance of the findings in relation to patient history and physical examination. Because hip pain is a common comorbidity of pelvic pain, knowing how to screen the hip joint for FAI or labral tears, rehabilitate hips with joint dysfunction, and help someone return to activity following a hip repair is valuable to the pelvic rehabilitation therapist.
As the athletic population may have increased risk of hip injuries due to overuse, traumatic injury, or vigorous activity, being able to address dysfunction in both high level and less active patients is necessary. Herman & Wallace faculty member Steve Dischiavi has developed a course rich in athletic examples and including education about activating fascial systems in various planes. If you are ready to step up your game related to Biomechanical Assessment of the Hip & Pelvis, check out this continuing education course taking place next in Durham, North Carolina in May.
If you area clinic owner, are in a management or leadership position, one of your jobs is making sure your therapists are using best practices. This can be a challenge when best practices are continually being researched and discussed, and when systematic reviews continue to tell us that pelvic rehabilitation research lacks homogeneity and enough high-level evidence to make convincing arguments about interventions. In the absence of this, we can still integrate recommendations from clinical practice guidelines and from best practice statements. The American Physical Therapy Association's (APTA) Section on Women's Health (SOWH) is participating in the APTA's initiative to develop clinical practice guidelines. For current guidelines, check out their page here. To see which guidelines are in development at the APTA, click here.

The American Urological Association (AUA) has also developed practice guidelines, including the Guideline on the Diagnosis and Treatment of Interstitial Cystitis/Bladder Pain Syndrome (IC/PBS). Within this guideline, the first line treatments are listed as general relaxation/stress management, pain management, patient education, and self-care/behavioral modification. Second-line treatments include "appropriate manual physical therapy techniques", oral medications, bladder medications (administered inside the bladder), and pain management. What is very interesting about this guideline is that the authors define what types of manual therapy approaches are appropriate, and these include techniques that resolve muscle tenderness, lengthen shortened muscles, release painful scars or other connective tissue restrictions. The guidelines also define who should be working with patients who have IC/PBS and pelvic muscle tenderness: "appropriately trained clinicians". Very importantly, the authors state that pelvic floor strengthening exercises should be avoided.
How can these guidelines be used to assess best practices? Find out if your therapists who work with patients who have IC/PBS are indeed instructing in relaxation strategies, using pain education and pain management techniques (for pain-brain education specific to pelvic pain, check out the book "Why Pelvic Pain Hurts". Find out if your therapist is instructing in pelvic muscle strengthening as a first-line of treatment, since this would not be in line with the AUA guidelines. (Having said this, teaching pelvic muscle strengthening can be very appropriate when done with consideration of pelvic muscle pain.) Lastly, ask your therapist if she feels that her skill set and training is sufficient to treat the condition. Even in our comprehensive pelvic floor series, there is so much to learn at the initial course that IC/PBS is not discussed in great detail until PF2B. Maybe a little more knowledge and training would help your therapist feel that she is providing the "appropriate manual physical therapy techniques" recommended in the guidelines.
To find out when the next intermediate or advanced course in the series is happening, or to find other specialty courses, check our course listings to see if there is a course happening near you!











































